Mr Gregg Alton
Executive Vice President of International Operations & Corporate Affairs, Gilead Sciences Inc.
cc: Clifford Samuel
Vice President of International Access Operations, Gilead Sciences Inc.
Dear Mr Alton,
On 16 February 2017, we wrote a letter requesting Gilead expand its not-for-profit price of liposomal amphotericin B (L-AMB) to include the indication of cryptococcal meningitis for low and middle-income countries (LMICs). We understand that, to date, Gilead has not provided the not-for-profit price for L-AMB for cryptococcal meningitis. Cryptococcal meningitis (CM) remains a significant cause of sickness and death among individuals infected with HIV: CM is responsible for about 15%-20% of all AIDS-related deaths globally.1 In the recently published ACTA trial, short course Amphotericin B deoxycholate (AmB) therapy was demonstrated to be powerfully effective in combination with flucytosine in people living with HIV who have cryptococcal disease, with a potential reduction in mortality to 24% [CI 16-32]. This is in the context of a background of 70% mortality for HIV-related meningo-encephalitis in many African LMICs.2 However, safe AmB deoxycholate administration requires a minimum package clearly outlined in WHO guidance for the prevention, monitoring, and management of toxicity to avoid the development of serious side effects due to AmB.1 This requirement precludes the use of AmB in many LMIC centers where it is often also unavailable or subject to frequent stockouts.
L-AMB, on the other hand, is associated with fewer side effects and does not require such monitoring, thus relieving already strained health systems in resource-limited settings. Clinicians with whom we work in South Africa report that up to a third of CM patients in routine care do not tolerate conventional Amphotericin B due to renal impairment and so cannot be provided with an effective treatment regimen. Additionally, it is associated with further reductions in mortality from cryptococcal disease due to the increased safety of the drug.3 LAMB has also been seen to be effective even at lower dosages; results from the Ambition trial demonstrated that a single large dose of L-AMB was well tolerated and highly effective as induction therapy compared to the standard 14-day course of L-AMB. These results have pushed the formulation forward to a phase III clinical trial, where a single dose of L-AMB on the backbone of two weeks’ fluconazole and flucytosine will be compared to one week of AmB deoxycholate and flucytosine.4
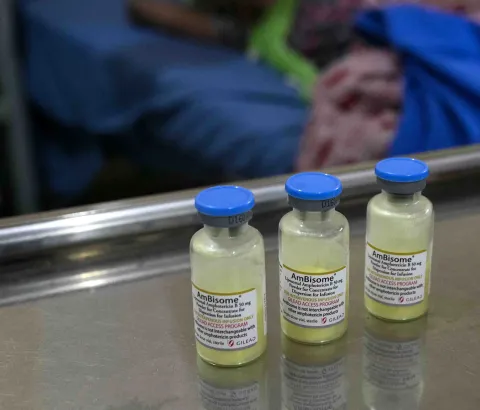
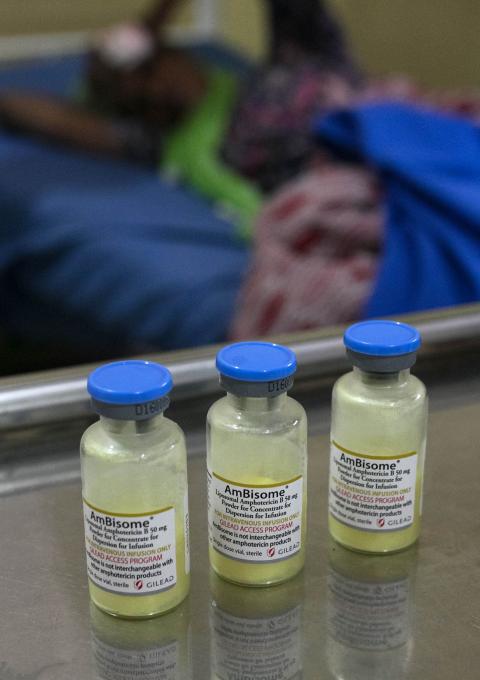
In its 2018 guidelines on the management of cryptococcal disease, the World Health Organization (WHO) recommended L-AMB as preferred treatment over AmB deoxycholate due to its equivalent efficacy and decreased side effects. Despite its clear safety benefits and efficacy at lower dosages, L-AMB was not recommended as the preferred first-line treatment due to high price.5 While L-AMB has been donated via WHO to six countries to treat visceral leishmaniasis, it is only currently available at full price (if at all), for the treatment of cryptococcal disease in LMICs where disease burden is highest.2 In South Africa, for example, LAMB is only available in the private market and sells at $212 per vial.6
Therefore, we are repeating our request that Gilead expands its $16.25 per vial price to all LMICs, NGOs, and public payers. Furthermore, as Gilead’s L-AMB has recently received approval from the WHO Pre-Qualification Programme, we request that Gilead expedite drug registration in high-burden countries through the WHO Collaborative Registration Procedure.
The need for L-AMB is stark and the potential benefits as a life-saving treatment for thousands of people living with HIV are clear. We look forward to hearing from Gilead regarding this request.
For further discussion, please feel free to contact Jessica Burry at MSF Access Campaign and Angela Loyse, chair of the cryptococcal Meningitis Action Group (cryptoMAG).
Sincerely,
Dr Angela Loyse
Senior Academic Clinical Lecturer
Honorary Infectious Disease Consultant
CryptoMAG chair
Jessica Burry
MSF Access Campaign
MSF Access Campaign
Mosepele Mosepele MD, MSc
Chair, Department of Internal Medicine, University of Botswana
Chair, Africa Meningitis Trials Network
University Teaching Hospital
Gaborone, Botswana
Dr Suzaan Marais
Consultant Neurologist
Inkosi Albert Luthuli Central Hospital
Durban, South Africa
Mina C. Hosseinipour, MD, MPH
Professor of Medicine
University of North Carolina at Chapel Hill
Scientific Director
UNC Project-Malawi
Timothée Boyer Chammard, MD
Infectious Diseases Physician and Clinical Researcher
AMBITION-cm clinical advisor
Molecular Mycology Unit, Institut Pasteur
Service des Maladies Infectieuses et Tropicales, Hôpital Necker-Enfants malades
Centre d’Infectiologie Necker-Pasteur
Paris, France
Olivier Lortholary, MD, PhD
Professor, Paris Descartes University
IHU Imagine
Service des Maladies Infectieuses et Tropicales, Hôpital Necker-Enfants malades, Paris
Centre d’Infectiologie Necker-Pasteur
Deputy Director of the National Reference Center for Mycoses and Antifungals
Molecular Mycology Unit, Institut Pasteur
Paris, France
Dr Douglas Wilson
Head of Internal Medicine at Edendale Hospital
Pietermaritzburg, South Africa
Nabila Youssouf, PhD
Ambiton-cm Trial Manager
London School of Hygiene and Tropical Medicine/ Botswana Harvard HIV Partnership
Princess Marina Hospital
Gaborone, Botswana
Dr Elisabeth Szumilin
HIV advisor, medical department.
Médecins Sans Frontières
Paris, France
Dr Nelesh Govender
National Institute for Communicable Diseases
South Africa
Dr Síle F Molloy
Centre for Global Health
Institute for Infection and Immunity
St George's University of London)
Jeremy Day MA PhD FRCP
Head, CNS-HIV Infections Research Group
Ho Chi Minh City Vietnam
Professor of Infectious Diseases
Centre for Tropical Medicine
Nuffield Department of Medicine
University of Oxford
United Kingdom
In partnership with
The Hospital for Tropical Diseases
Ho Chi Minh City
Dr David W. Denning
Chief Executive
Global Action Fund for Fungal Infections
Geneva, Switzerland
Professor of Infectious Diseases in Global Health
University of Manchester
Professor Thomas S Harrison
Centre for Global Health
St Georges University of London
Jennifer Cohn, MD MPH
Assistant Professor, Division of Infectious Diseases
University of Pennsylvania
Juan Luis Rodriguez Tudela, MD, PhD
Senior advisor for GAFFI
Genève, Switzerland
Ms Philippa Griffin
Financial & Administrative Project Manager, EDCTP-funded AMBITION
London School of Hygiene and Tropical Medicine
David Lee Chin, MD
Director Technical Strategy & Quality
Pharmaceuticals and Health Technologies Group
Management Sciences for Health
Arlington, VA
Henry C Mwandumba, MBChB (Hons), DTM & H, FRCP (UK), FCP (ECSA), PhD
Deputy Director, MLW
Reader & MRC/DfID African Research Leader
Consultant Physician in General (Internal) Medicine & Infectious Diseases
Malawi-Liverpool-Wellcome Trust Clinical Research Programme (MLW)
Malawi
Joseph Jarvis
Professor of Tropical Medicine and International Health
London School of Hygiene and Tropical Medicine
Dr Cecilia Kanyama
Physician Investigator
UNC Project
Lilongwe. Malawi
Prof Dr Sayoki G Mfinanga,
Chief Research Scientist and Director
Muhimbili Medical Research Centre National Institute for Medical Research (NIMR)
Professor of Global Health: Liverpool School Tropical Medicine,
Lecturer: Muhimbili University of Health and Allied Sciences
Graeme Meintjes
Professor of Medicine
University of Cape Town
Thuy Le, MD, DPhil
Associate Professor of Medicine (pending)
Division of Infectious Diseases and International Health
Duke University School of Medicine
Oxford University Clinical Research Unit in Vietnam
In partnership with the Hospital for Tropical Diseases, Ho Chi Minh City, Vietnam
David Meya
Associate Professor
Infectious Diseases Institute
Dr Duncan M Chanda
Physician/Infectious Diseases Registrar
University Teaching Hospital
University of Zambia School of Medicine
Lusaka, Zambia
References
1World Health Organization. (2018). Guidelines for the Diagnosis, Prevention, and Management of Cryptococcal
Disease in HIV-Infected Adults, Adolescents, and Children.
2Rajasingham R, Smith RM, Park BJ et al. Global burden of disease of HIV-associated cryptococcal meningitis: an updated analysis. The Lancet, Infectious Diseases. 2017 May; 17(8): 873-881. Last accessed 28 June 2018.
3Bicanic T, Bottomlet C, Loyse A et al. Toxicity of Amphotericin B Deoxycholate-Based Induction Therapy in
Patients with HIV-Associated Cryptococcal Meningitis. Antimicrobial Agents and Chemotherapy. 2015 Dec;
59(12):7224-31. Doi: 10.1128/AAC.01698-15. Epub 2015 Sep 8.
4Jarvis JN, Leeme TB, Chofle AA et al. Ambition-CM: High dose liposomal Amphotericin for HIV-related
cryptococcal meningitis [abstract]. In: Conference on Retroviruses and Opportunistic Infections; February 13-16,
2017; Seattle, Washington. Abstract number 82. Last accessed 28 June 2018.
5World Health Organization (2017). Guidelines for Managing Advanced HIV Disease and Rapid Initiation of
Antiretroviral Therapy. Last accessed 28 June 2018.
6Medicines Price Registry, South Africa. Accessed online, 4 July 2018.