Cryptococcal meningitis: This World AIDS Day it’s time to recognise an outsider
Opinion piece by Dr Amir Shroufi*
Outsiders seldom get the attention they deserve. When it comes to conservation, for example, a few popular species attract most of the available funding – the rhino overshadows riverine rabbit. In the arts, jazz and blues struggle to attract the attention given freely to catchy pop, and it’s rare to see a documentary, however deserving, surpass the success of an action film at the box office.
It can be difficult to pinpoint why this sort of thing happens but the phenomenon extends to diseases too. A difficult and academic sounding name does not help a disease gain widespread recognition. Some diseases mostly affect people living in low and middle-income counties, leading pharmaceutical corporations to view them as unprofitable (often a misperception). As a result, money doesn’t flow into needed research and development for treatments, in turn hampering the engagement of the wider scientific community.
Cryptococcal meningitis, which fits all of the criteria above, is a notable disease outsider, despite being responsible for an estimated 180 000 deaths annually, mostly of people under the age of 40 living in sub-Saharan Africa.
The causative agent, the cryptococcus, is everywhere in the environment. For those of us with a fully functional immune system it causes no harm. However, in people with HIV who have severe immunosuppression it can invade the lining of the brain, quickly leading to severe disease and death if left untreated.
This grim picture may lead you to think that cryptococcal meningitis is incurable, but this isn’t the case. In fact, with early diagnosis and optimal treatment, mortality could be reduced by over 70%. Achieving this at the population level, by ensuring everyone with the disease was managed well, would help to avert hundreds of thousands of deaths between now and 2030.
This is far from the current reality and it is a marker of the lack of recognition given to this disease that life-saving tools developed decades ago are still barely used today. Flucytosine - an essential drug for the treatment of cryptococcal meningitis - was developed in the 50s, is off-patent and is very simple to make. Yet, most people with the disease today will never access it. There are many reasons for this lack of access: funding challenges, low clinical awareness and a need for training. The other big reason why flucytosine is rarely used is the fact that it is not registered in most countries where it is needed. On World AIDS Day 2021, it is time for countries to address that.
In South Africa, for example, while registration has been in process under the South African Health Products Regulatory Authority (SAHPRA) for almost 2 years, it has still not been finalised. SAHPRA should urgently proceed to register this medicine, following which the government of South Africa has an opportunity to rapidly ensure all of its people who need it can access this life saving medicine by rapidly rolling out supplies and necessary support.
Cryptococcal meningitis and the bigger HIV picture
Scaling up antiretroviral therapy is by some way the most important means of improving the lives of people living with HIV (PLHIV) and addressing the AIDS epidemic, but it is not by itself enough. In 2019, there were still 690,000 deaths from HIV-related causes, including from opportunistic infections like cryptococcal meningitis. Improving things on the treatment side of the equation could help address that.
In HIV care, a public health approach and quality care for the very sick have for too long been pitched as mutually exclusive. It is time to focus proportionate energy and investment on PLHIV who become sick with opportunistic infections, ensuring that they get the care they deserve.
What needs to change?
There is a global strategy to end tuberculosis, the biggest killer of PLHIV, but no strategy to end cryptococcal meningitis, nor other major causes of death of PLHIV.
UNAIDS and the WHO, the multilateral health organisations at the helm of the HIV response, can help by acknowledging the seriousness of the problem through steps that include measuring cryptococcal meningitis deaths, setting targets for reducing those deaths, and helping countries develop strategies for meeting those targets.
It is regrettable when an outsider doesn’t receive due recognition. In the case of cryptococcal meningitis, it’s an avoidable tragedy
* Amir Shroufi is a former MSF South Africa medical coordinator and current member of the MSF Southern Africa Board of Directors. He is a UK-trained medical doctor and has completed post-graduate specialist training in public health. Following an early career in acute medicine, he has spent the last 15 years working in public health. For the last 10 years, he has worked on programmes addressing HIV and TB in Southern Africa, most of that time working for MSF, including as the medical coordinator for MSF in South Africa, where he helped to establish stop stockouts project and the South African Flucytosine Access programme. Amir current works as a medical advisor for the Centres for Disease Control and lives in Cape Town.
Testimonies
Dr Rosie Burton*, MSF infectious diseases physician
Three considerations to treat or manage CM
Point number one is that opportunistic infections like cryptococcal meningitis are still killing people who are living with HIV. We start a lot of people on antiretroviral therapy (ART) now, but it is important to note that ARVs is not the only strategy required, we also need to be rapidly diagnosing and optimally treating opportunistic infections. Cryptococcal meningitis is an opportunistic infection that also has a very high mortality. So I think that's the first point, that it is not over, a lot of people still die of HIV-related causes.
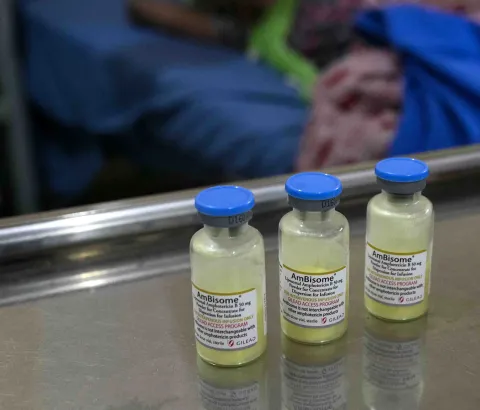
Point number two is that it's important to start treatment at diagnosis with the best treatment that is available. Cryptococcal meningitis is a neurological disease, so it affects the brain, and any disease affecting the brain is serious. People suffering from it may be quite well at diagnosis - diagnosed not on account of their symptoms but because they happened to receive a test. Probably they may be seriously ill and unconscious. There may be nerve problems, like eye movements, or even an inability to see, and these are manifestation of a high level of pressure inside the brain. Therefore, patients require early diagnosis followed by immediate initiation of the best treatment available. In terms of medical treatment, having access to a drug called flucytosine means we can give the partner drug, which is amphotericin B, for one week rather than two weeks, which reduces the risk of side effects from amphotericin B. We know that treating with flucytosine compared to fluconazole – the drug that is most often used in partnership with amphotericin B when flucytosine is not available - improves mortality. It saves lives, and also reduces hospital time. Flucytosine is available in all of our MSF projects, where we would routinely use flucytosine with amphotericin B for one week, which is in contrast to the South African healthcare system currently, where outside of clinical trials it's still two weeks of amphotericin B usually with fluconazole. Flucytosine greatly simplifies and shortens medical treatment, which is why MSF has been pushing for its speedy registration for use in South Africa and elsewhere.
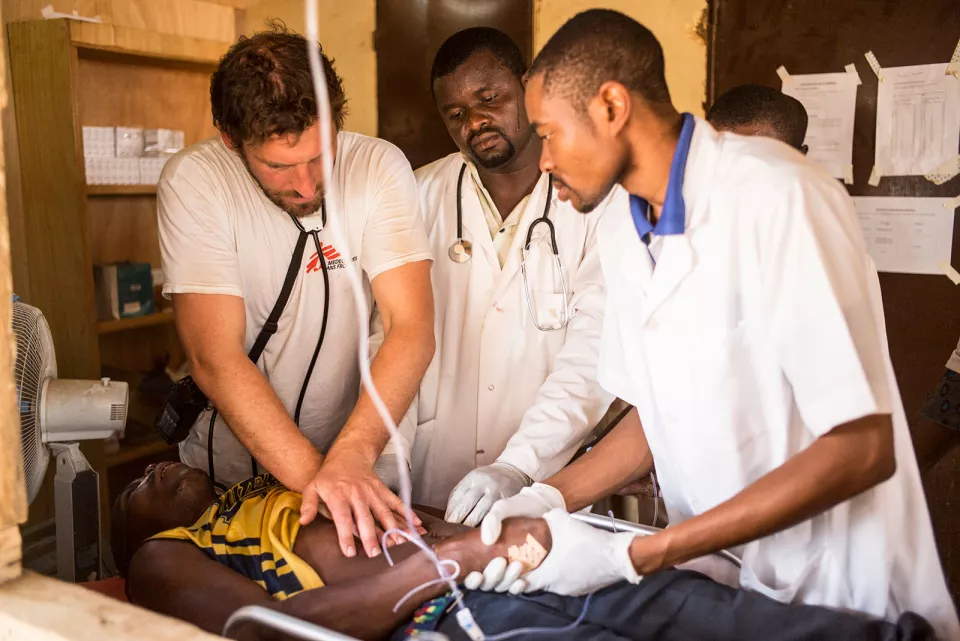
The third thing to emphasise is that it’s not just medical treatment that is required - the role of the lumbar puncture to relieve pressure on the brain is of critical importance, and patients need hospitalizing with medical or nursing teams who've just had training on lumbar puncture. Patients with cryptococcal meningitis often get worse before they get better. It’s not a disease where people start getting better from day one. They need a lot of medical care to see if they're deteriorating, which is usually because of raised intracranial pressure, which we then manage by doing more lumbar punctures. In my view this is not always done as aggressively as it should be. Sometimes people say, "well, the patient doesn't have any symptoms today,” and yet you find the pressure was high yesterday, so you must do the procedure again. The impacts can be dramatic. I had a patient recently in Bangui, in the Central African Republic (CAR) who had seizures, and he was unconscious. We did a therapeutic lumbar puncture, but we were feeling he probably wouldn't make it. A few hours later he was awake again, and when we arrived in the morning he just said, “Oh, hello.” So it's not just the medical treatment that is important - you need the whole package of care.
* Dr Rosie Burton has cared for cryptococcal meningitis patients in several countries across West, Central, East and Southern Africa.
Zikhona Mboto
I was diagnosed with HIV in 2018. By the beginning of 2019 I was vomiting up some of my antiretroviral drugs (ARVs), but I never reported that to the clinic because I thought it was normal. I started having headaches, not just normal headaches… serious headaches. I couldn’t even sit or sleep. The headache would pound anytime…night, day. Sometimes, at first, the pain would disappear for an hour maybe, then it would come back. I took Grandpa (paracetamol) but it didn’t help, so I decided to go to the doctor. The doctor told me it was low blood pressure, not too serious, and I went back home. But it continued and now I was at a point where I had blurred vision. My relatives were advising me to see a sangoma (a traditional healer). You see, when something like this happens in our culture, when it feels like boiling blood has been poured into your brain and paracetamol doesn’t help, some will believe that there has been foul play, and you must see a traditional healer. My aunt who is a nurse in Mitchell’s Plain, in Cape Town said “no, she is going to hospital now,” and when I was trying to get out of bed I had a seizure, and I only woke up the next day in hospital. They did a lumbar puncture (a medical procedure in which a needle is inserted into the spinal canal), and then they told me that I have cryptococcal meningitis. I was like, “what is cryptococcal meningitis?” And they explained that it's when your brain is attacked by a certain bacteria, and it puts pressure on the brain.
I was terrified. When it has to do with the brain, you get scared. I thought I was going to die, because I was still vomiting up medication, so I was wondering how am I ever going to get healed? The only time I felt some relief from the headache was when they did a lumbar puncture, and as painful as this procedure is, I would call the nurse and ask for it, as many as three times a day. I was on a drip, and they included me in a clinical trial and I received flucytosine as part of my treatment. This is an antifungal medicine that is not available normally, so I was fortunate. I was discharged after 14 days, and although they said the infection was clear, I felt sick when I got home, so I was admitted for another seven days for observation. The headaches are clear now and I can get back to my normal life.
What I want to say to others is you need to take your ARVs properly. If you don’t it leaves the gate open for opportunistic infections like cryptococcal meningitis. When I was diagnosed with crypto, my CD4 count was as low as one, I had no immunity. Now I make sure that I take my treatment correctly.
My other message is don’t wait to go to hospital. I had symptoms of cryptococcal meningitis already in December 2018, and I was diagnosed in March 2019. Waiting almost cost me my life.