Why is it so difficult to achieve and sustain high levels of immunisation coverage in remote areas, or where health systems are severely limited? Dr Michel Quéré, MSF medical advisor for programmes in Niger, Chad and the DRC, explains why the vaccines at our disposal today make reaching remote populations considerably more difficult.
Our catch-up vaccination programmes are quite successful – the idea is to give children the vaccines they have missed, for example against measles or the pentavalent vaccine. We get good results because we put a lot of effort into raising awareness in the community, explaining which age group will get vaccinated when and why that’s important, and our locally recruited nurses play a vital role.
But it’s definitely the case that we get good results also because we have considerable logistical support at our disposal. We’ve got the large storage facilities, the fridges and icepacks to keep the vaccines under cold chain, the transportation to get them out to the villages and the logisticians to make sure that it all runs as smoothly as possible.
With some vaccines, children need to receive several doses, several months apart to receive full protection. That means, for instance, to make sure a child is fully protected with the pentavalent vaccine, you have to trace the child on three separate occasions so that they can receive three doses of the vaccine. And if you’re also giving additional vaccines, then the ages at which you need to vaccinate don’t necessarily coincide, so for every child under the age of one, five separate visits may be needed.
Reaching children scattered across the absolutely vast and remote areas where they live is a real challenge – the roads are usually very bad, and some of the health posts – for instance in the Democratic Republic of Congo – are so isolated, or present such security concerns, they can only be reached by plane.
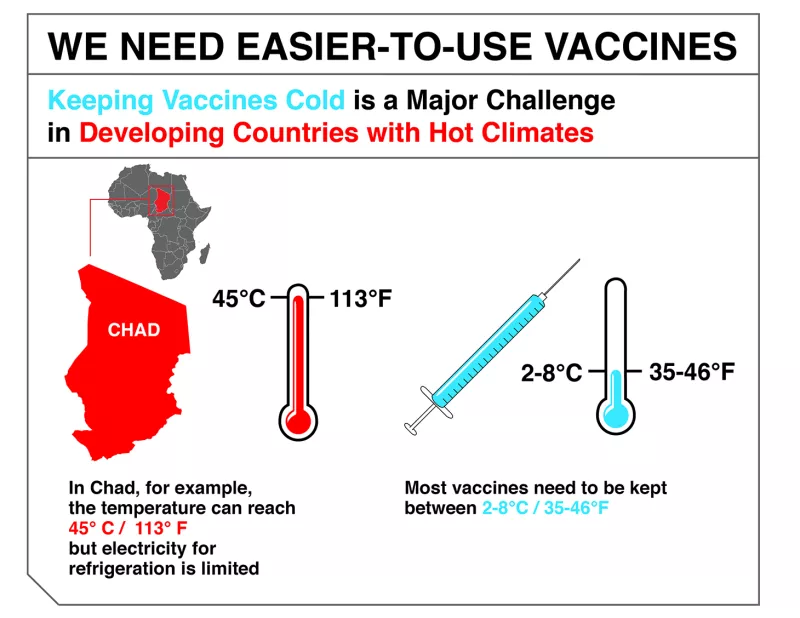
Keeping the cold chain when it’s 45˚C outside is a major challenge. For the national health authorities, in some rural areas, just maintaining the fridges in working order is hard to guarantee, and then there’s the need to produce enough ice packs so that the vaccines are still cold by the time we get to the children. You can imagine how many icepacks are needed, so even getting the vaccines out to the villages is a huge logistical effort in itself.
The governments or local authorities rarely have the means at their disposal to get all this done – there might be only one nurse available, expected to provide services for 10,000 people and that number can go up to 50,000 people in some parts of Niger and he or she will often have no means of transportation.
So it’s very clear that we need things to be made simpler. A vaccine that can be taken orally is ideal. It can thus be administered more simply – even by community health workers – and so can be made available much more widely, overcoming the shortage of health staff. We also need to get around the problem of needing a cold chain as it’s a huge burden in terms of resources.
Unless vaccines are simplified so that they’re better adapted to real-life conditions, we will never get on top of these killer diseases and will always need to respond to outbreaks that we haven’t managed to prevent through effective immunisation programmes.
Sadly, there’s been little progress in this regard over the last 20 or 30 years. And unless we see some changes, we’re not likely ever to achieve the goal of good EPI coverage. Adding new vaccines to the mix isn’t going to bring us closer to achieving that goal either.
It might cost more to develop and provide better-adapted tools, of course. But responding to epidemics and disease outbreaks is hugely costly, and children who are ill become vulnerable to other conditions like malnutrition, so the extra expense should quickly be offset with other gains. That’s putting to one side the fundamental question of whether you can put a price on saving a child’s life.