"I didn't want to believe it," 24-year-old Arzubay recalls, describing his experience being diagnosed with multidrug-resistant tuberculosis (MDR-TB) in 2013. "I wanted to ignore what the X-ray film had shown by saying that maybe I swallowed a gulp of air into my lungs when the X-ray was taken. I was ambivalent, and submitted sputum (fluid from the lungs) twice for lab analysis. But when doctors confirmed the diagnosis of TB, there was no way to get out of the situation."
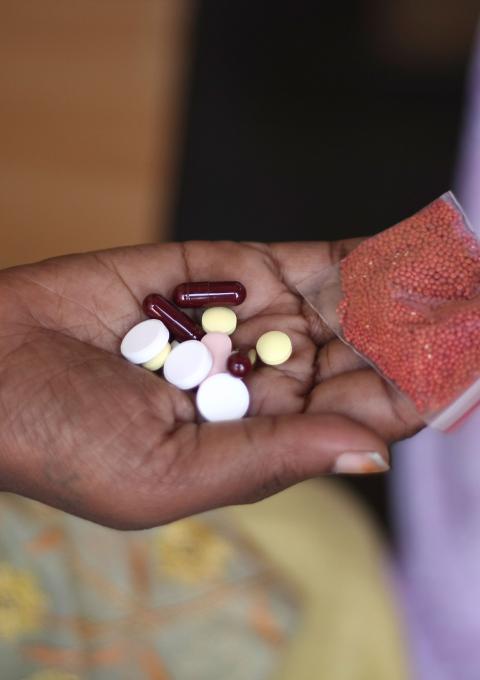
It is no surprise Arzubay was not ready to accept the diagnosis: It was the first time he was diagnosed with TB and it was MDR-TB, a form of the disease that does not respond to first-line TB drugs. He wondered how that could have happened. Customary treatment for MDR-TB lasts for about two years, while a course of treatment for uncomplicated tuberculosis takes about six months. During the course of MDR-TB treatment, patients have to take more than 10,000 pills and have painful daily injections for at least eight months. Side effects from treatment are often intolerable, and include continuous severe headache, nausea and joint pains; mentally, it is difficult to bear the treatment for such a long period.
Arzubay was diagnosed at Kegeyli district TB dispensary in Karakalpakstan, an autonomous republic located in the northwest of Uzbekistan. It has the highest number of TB cases in the region, where Médecins Sans Frontières (MSF) runs a programme offering TB treatment to more than 2,000 patients with drug-sensitive (DS), drug-resistant (DR) and extensively drug-resistant (XDR) forms of TB.
In 2013, MSF and the Ministry of Health of Uzbekistan initiated a study to evaluate the effectiveness and side effects of a simplified short-course regimen (SCR) for treatment of MDR-TB, which reduces the duration of treatment by more than one year. For patients like Arzubay, this meant a light at the end of the tunnel and alleviated some fears of facing two years of arduous treatment.
Patients who qualify for the SCR take treatment for a minimum of 9 and maximum of 11 months. At the beginning, the treatment regimen requires that patients receive painful injections of high-dose isoniazid for at least 4 months and no longer than 6 months. After that, patients are transferred into a treatment continuation phase for five months, which serves to improve treatment tolerance.
Arzubay was one of the first patients enrolled in the study. "The medical team introduced SCR and the doctor told me I met the criteria," he says. "I started my treatment in September 2013. I felt so happy being offered SCR, because I already knew some people were struggling with two years of treatment and I also saw the ones who had no other treatment options left. Besides, nine months was not so long for me, and didn't keep me from helping my family with daily chores. I didn't have to make a choice between supporting my family and getting cured."
Dr Marjan, Arzubay's doctor, says Arzubay is "...the best example of the successful implementation of the TB programme in Kegeyli district." Marjan is optimistic about the results of the study: "Overall, we observed that patients undergoing SCR have fewer side effects. Of course, we treat each patient individually. What is good about SCR is that patients can go back to their previous social life in a short time. I can see that from the examples of patients when they ask me if it is ok to work, or even go abroad."
Due to the success of this study, and following new WHO recommendations that include the SCR, the Karakalpak Ministry of Health is now using the SCR as part of the locally accepted conventional treatment regimen. September 2017 marked three years since Arzubay completed SCR treatment. He is doing well, with no signs or symptoms of TB. He sees a TB doctor for a regular check-up once a year. At home, he helps with farming – and he also found a job he likes in a railway station as a rail loader assistant.
"It is good that SCR treatment is made available for people like me. Now they don't have to be afraid of the treatment challenges. For me, the last months of treatment (the continuation phase) became easier to tolerate when [doctors] took out injections and isoniazid. Moreover, support from peers at the 'DOT corner' and doctors, nurses and cousellors just added value to my wish to be cured soon," says Arzubay.
Having been through TB treatment himself, Arzubay understand the challenges faced by people with TB. From time to time on his way to work, he visits the 'DOT corner', where he used to take his medicines, to talk with patients and share his experience.
Médecins Sans Frontières has been treating people with TB for 30 years. In 2016, MSF treated more than 20,000 people with TB, including 2,700 people with MDR-TB.
MSF has worked in Uzbekistan since 1997 and continues to work towards improving the quality and availability of TB treatment. MSF now focuses on providing care to people with MDR-TB due to the high burden of the disease in the country. In 2016, over 2,646 patients started TB treatment in this programme; 1,767 were treated for DS-TB, and 878 for DR-TB.
In July 2016, MSF began treating children with DR-TB on a shorter treatment regimen of nine months, instead of the usual 12 months or more, and has been conducting research into the results. MSF also investigated medical outcomes for adults on the shorter treatment. Recently, MSF launched a new clinical trial in Uzbekistan to develop a radically improved course of treatment for DR-TB. The first patients enrolled in the trial, TB PRACTECAL, began treatment in January 2017. The trial combines the first new TB drugs available in over 50 years with existing drugs to develop shorter, more tolerable treatment regimens.
