You’ve done several missions with MSF as a nurse. Looking back, do you remember encountering any kids with pneumonia?
In our work, we see so many children with respiratory infections. After several missions with MSF, it’s very common to see — kids either come in because of diarrhea, malaria, pneumonia, or some kind of combination of these three. When I think about it, I actually remember the first baby I ever saw with pneumonia was on my first mission with MSF. We were in Colombia setting up mobile clinics in remote areas, which would take around 6 to 8 hours by canoe to reach. Our national staff — doctors and nurses — would do the medical consultations, and the expatriate staff was there to help. I was there to triage, so I assessed the patients as they came in and give a quick diagnosis of each case.
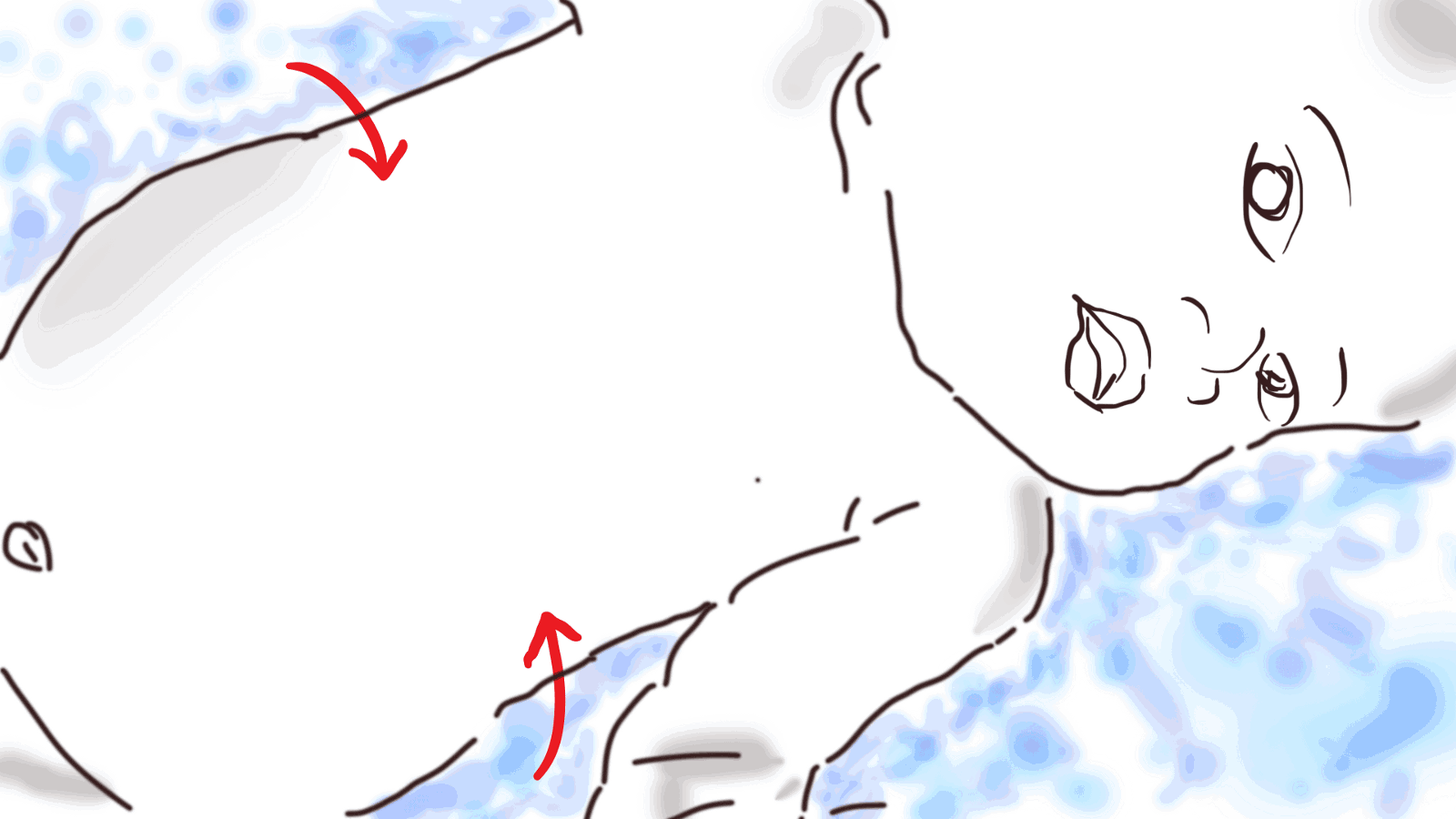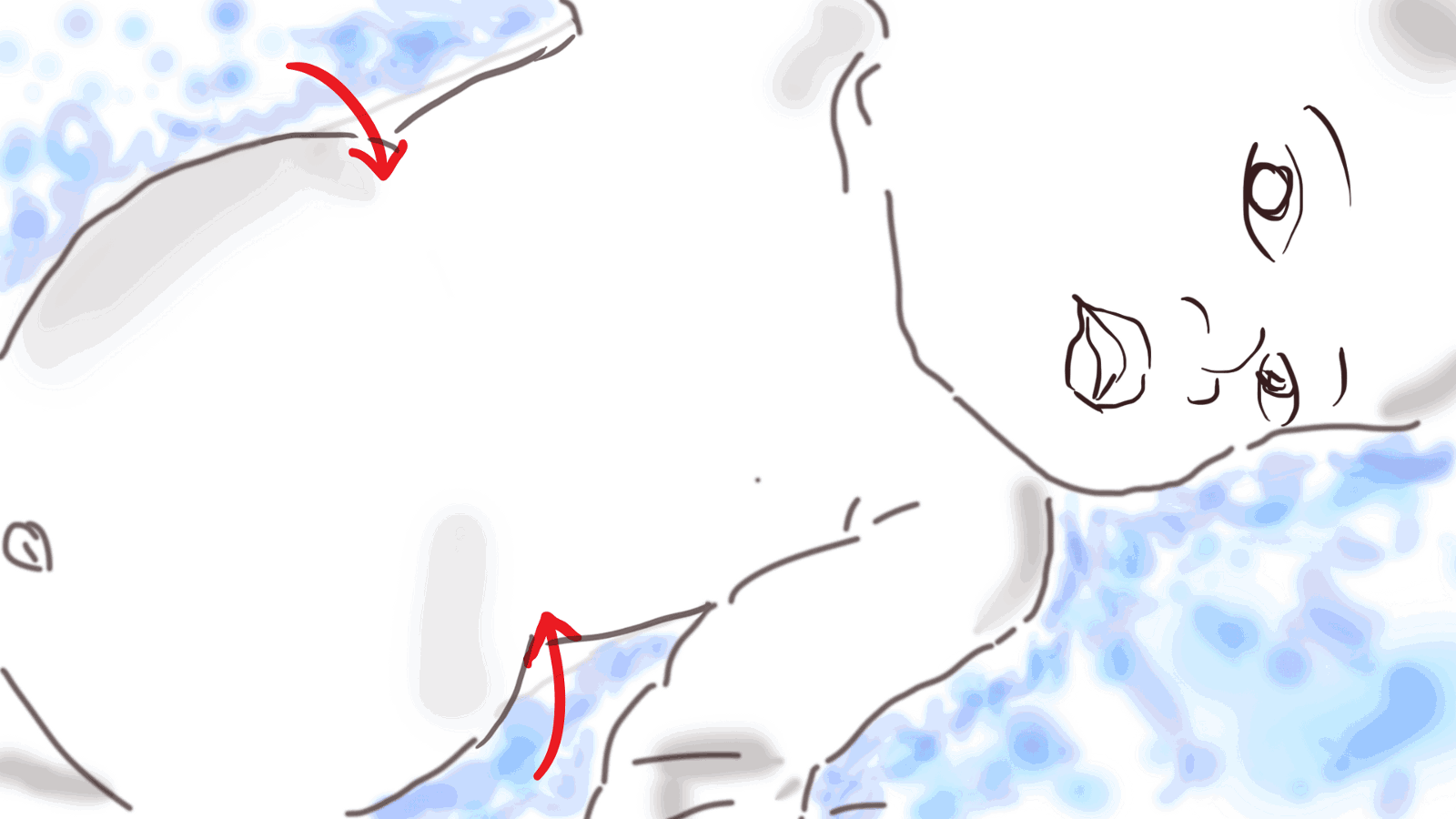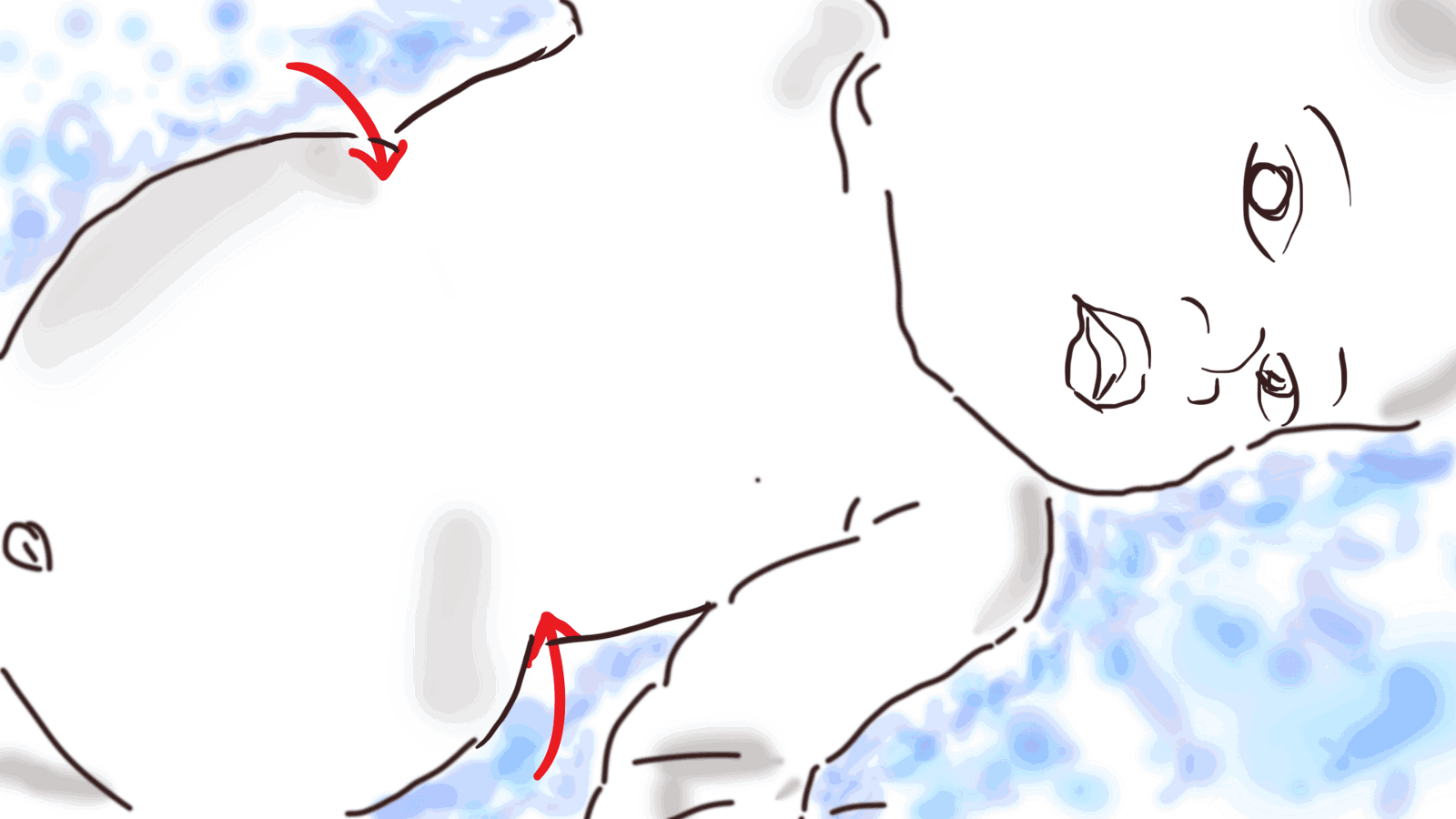
I remember this baby on our second-to-last day of the mobile clinic. There was this mother with her baby, and I thought the baby was very small, maybe 8 months old. He had the classic chest in-drawing, but at that time in my life, I was not so used to seeing it. I didn’t know immediately what it was. He had such a difficult time breathing; gasping for air, the chest draws very deeply inwards. You really can see the ribs contract, because his body and lungs were trying to get as much oxygen as they could. The baby was completely dazed, not crying…
What did you do then?
I went to the doctor and said, “There’s this child… he’s breathing so weird.” And the doctor said to bring him to her immediately. I told the mother to come, and I stayed to observe because I saw how worried the doctor was. The doctor had worked her whole career in this context — helping underserved people — and to see her so concerned was alarming. It took me a while before I understood that the baby had pneumonia. And I really felt bad afterward, because I didn’t think the baby was in as bad of a condition as he was. I told you, I never saw any child come in with that kind of sickness before.
When you were practicing as a nurse in Italy, you never saw a child like that?
No, no. In Italy, most of the kids are vaccinated against pneumonia. And if they do get sick with respiratory illnesses, the access to healthcare is pretty good and we can treat the child early.
What’s the biggest difference between a pediatric ward in Italy and one in an MSF setting?
There’s no crying in the pediatric wards in MSF settings. There is no sound. Maybe just the normal sounds of a clinic, like the nurse walking or maybe the sound of a mother. It is not a pediatric ward as you imagine. When kids are very sick, they don’t really cry. It is very striking, because one of the serious signs of how sick a kid is, is when they don’t cry. Or when they cry without tears.
It’s crazy how, depending on where you’re born, your chances of survival can vary so greatly. What happened to the child in Colombia?
Once the baby was with the doctor, we ran several tests. We were worried because he was so listless. After that, it was clear that the baby needed to be referred to the hospital which was 6 hours by canoe and 4 by car, we kept the baby under observation overnight. Luckily we had a small oxygen tank with us and we could keep the baby oxygenated, I am telling you not an easy task to safely transport oxygen tank in a mobile clinic.So this story went very well because we were also leaving the next day. The mother and baby came with us and we traveled in the canoe for 5 to 6 hours. When we reached the village called La Gabarra, from there we had our MSF cars. Everyone jumped in the car and we brought the mother and baby to our base in Tibu, which was 4 hours (with good weather condition) by car from La Gabarra. Once we arrived in Tibu, the ambulance was waiting for us to bring the baby to the state capital hospital, another 4 hours by the road. That went very smoothly and the baby was fine. We did these mobile clinics every two weeks, so afterward we were able to follow up and check up on him.
That’s good news.
Yes, we were very lucky, because he must have been very sick for at least a week before he came into our clinic, but the family wasn’t able to seek healthcare sooner. I say this completely without judgment because you have to understand the setting. It’s not easy to reach healthcare in these areas. Like I said, it takes hours to travel by canoe and car to reach the nearest hospital. And you need money to pay for transportation, to pay for the canoe, then the car, and journey back. It’s not easy.