Dr Séverine Caluwaerts is a Belgian obstetrician/gynaecologist who has worked with Médecins Sans Frontières/Doctors Without Borders (MSF) in maternal health projects including in Sierra Leone, Burundi, Democratic Republic of Congo and Afghanistan.
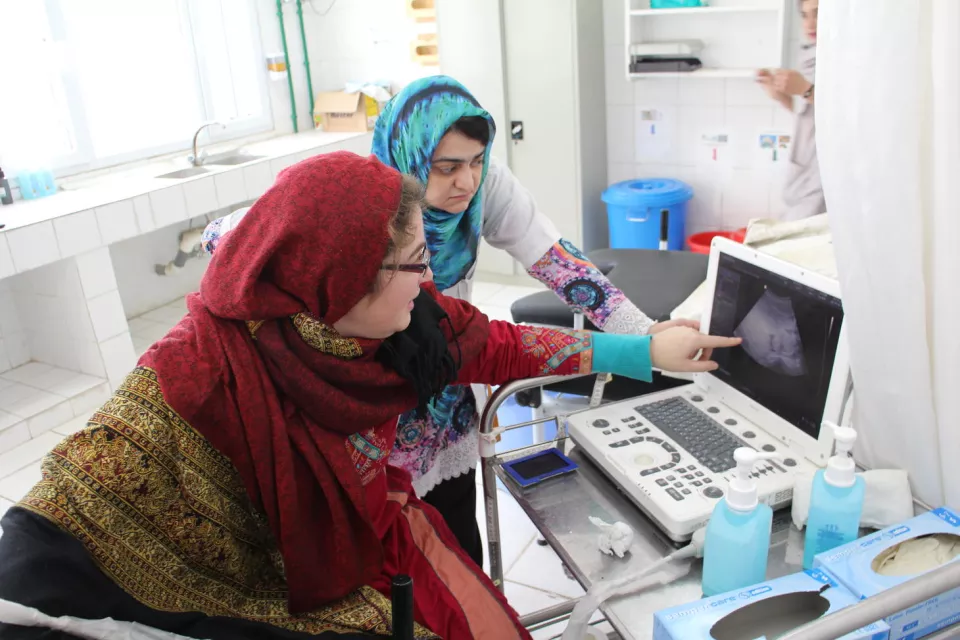
Two years ago, I travelled to Maputo, Mozambique to help the team with cervical cancer screening activities, and to help address difficult cases and other challenges. In Maputo, MSF is focused on screening HIV positive women because they are most at risk of developing cervical cancer. The HIV epidemic is rampant here and although one in eight women lives with the virus, lifesaving antiretroviral treatment has become far more accessible in recent years.
Together with the friendly nurses, I’d been following the sexual and reproductive health consultations the entire morning. The nurses and patients laughed at my limited Portuguese but somehow, they managed to understand me. Women consulted for various reasons at this clinic; I saw around 20 women and girls come in for HIV testing, family planning, for their first antenatal care visit and cervical cancer screening. Sometimes patients consulted for HIV testing, family planning and cervical cancer screening all in the one visit.
Forty-year-old Maura* came in, our last patient of the morning. I immediately notice how thin she is and the swollen lymph nodes in her neck. “Benvindo Maura,” I say, “Sou doctora Séverine do MSF.” I get a warm smile in return. The nurse asks Maura why she has come into the clinic today. “I have belly pain,” she says, “and there is something dirty coming out of my vagina.”
I instantly hope that this is ‘just’ a sexually transmitted disease, something treatable. But during the examination, the nurse and I see a large mass coming from the cervix, protruding into the vagina. Further examination reveals that the mass extends to the pelvic wall.
After she is dressed again, we counsel Maura for HIV testing. She agrees and, as we suspected, she tests positive. The nurse sits down with Maura and explains very gently that she has two serious conditions – cervical cancer and HIV. The nurse reassures her that we will do everything we can and that she will be referred to the HIV clinic and can start treatment as early as today.
The treatment for her cervical cancer, however, is complicated. It’s inoperable and she needs radiotherapy to have any chance of survival. There is no radiotherapy unit in Mozambique, so patients are referred to hospitals in South Africa, but in reality, this system is not functioning because it is too far, too expensive and too complicated.
Two years ago, I hugged Maura, wished her all the best and went home with a sick feeling in my stomach. Maura’s serious health issues were largely preventable. If only she could have come for screening, if only she had had her HIV test sooner. If only…
Today, more women die worldwide of cervical cancer than of complications of pregnancy and delivery. In 2018, 311,000 women died of cervical cancer and these were mainly women living in low-income settings with limited financial, cultural or geographical access to quality medical care.
The figure is projected to increase in coming years, yet the world is largely silent about these deaths. The worst part is that preventive tools including human papillomavirus (HPV) vaccination and treatment like cryotherapy (freezing of the cervix) are available and, in the case of the latter, affordable.
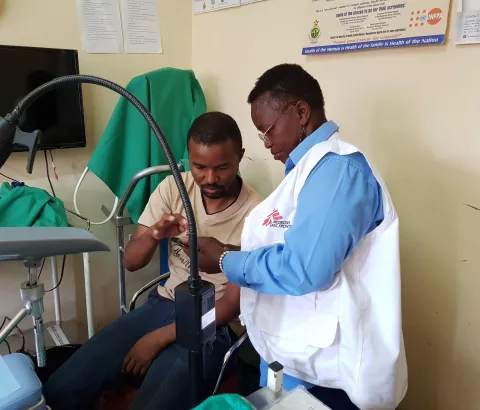
Last July, I travelled to Zimbabwe where MSF is managing a cervical cancer screen-and-treat programme in collaboration with the Ministry of Health and Child Care. The screening is integrated into six clinics where women also receive family planning, HIV testing and treatment if needed. The team screened 5,751 women in Gutu district last year, and we’ve now reached 75 per cent of the women in the catchment area. We do health promotion in the clinic and we invested in Loop Electrosurgical Excision Procedure, to be able to better treat precancerous lesions that we detect using VIA (visual inspection of the cervix with acetic acid).
All this has brought good results. Year after year, more women come for screening and we detect fewer abnormalities. Perhaps this is due to a combination of more women being screened earlier, our teams doing outreach, and staff being better trained to recognise abnormalities. We also know that long-term effective HIV treatment helps to spontaneously clear precancerous lesions.
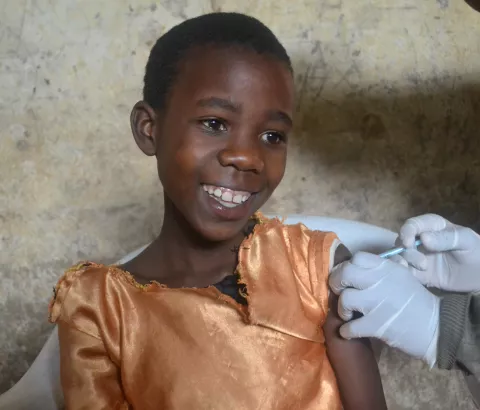
Last year in Gutu, MSF also carried out an HPV school vaccination campaign for 9-10-year-old girls, and supplied vaccines for 1,000 HIV-positive girls and young women aged 15-26. This vulnerable patient population now has a very good chance of life-long protection against this deadly disease.
So, by vaccinating young girls and by providing on the spot screening and treatment, we give more than just hope – we prevent cervical cancer from developing – so more women like Maura have a chance to survive.
But so much more needs to be done.
*Patient’s name has been changed to protect confidentiality.