MSF expands treatment for people living with HIV, including the “Gold Standard” of treatment monitoring.
Viral load testing shows the amount of HIV in the blood of a person living with the virus. Antiretroviral drugs suppress HIV replication. If a person on ARV treatment has a viral load above a certain point, it indicates that the treatment isn’t working,either because the medicines aren’t being taken correctly, or that HIV has become resistant to the antiretroviral medicines.
In either case, health workers can respond quickly, working with people on treatment to improve adherence to a drug regimen or prescribing advanced ‘second-line’ drugs. These steps can bring viral load down to virtually ‘undetectable’ levels, helping those on treatment stay healthy and benefiting the community by reducing the risk of transmission. Sexual transmission of HIV is 96% less likely when viral load is undetectable.
Viral load testing is the gold standard for monitoring the health of people on HIV treatment. But because the equipment can be expensive and requires skilled staff, the test is not widely available in poor countries with limited resources.
MSF – thanks to co-funding from UNITAID – is working to develop ways to expand viral load testing in eight countries in sub-Saharan Africa, including MSF sites in the Democratic Republic of Congo, Lesotho, Malawi, Mozambique, South Africa, Swaziland, Uganda and Zimbabwe. These pictures offer a glimpse of MSF viral load and HIV treatment projects in Malawi, where the HIV adult prevalence is high at about 14-16%.
A health worker at Bvumbe Health Centre in Malawi’s Thyolo District dispenses antiretroviral medicines. If a test shows a high viral load, treatment counsellors can intervene to help people living with HIV take medications on schedule - or, if appropriate, prescribe advanced medicines. “I know the drugs are working in my body with viral load testing,” said one person on treatment, who came to pick up test results.
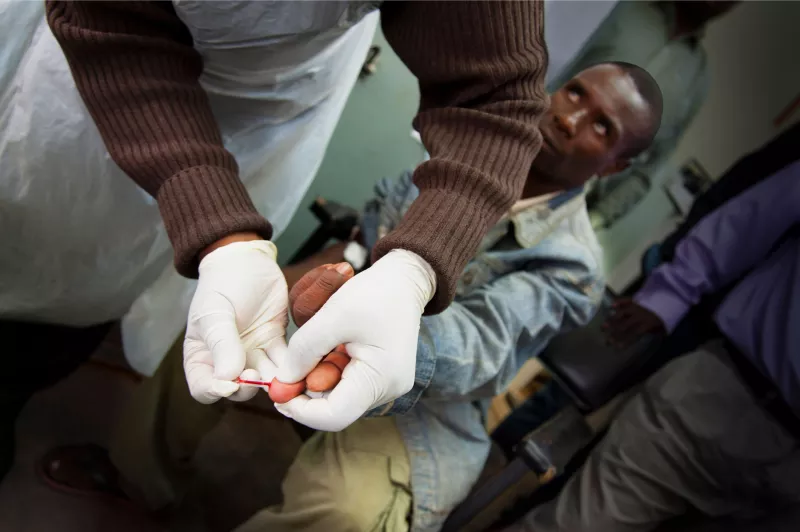
A community health worker at Bvumbe Health Centre pricks a man’s finger for a sample used in a dried blood spot (DBS) viral load test. An MSF study in Malawi found that samples gathered this way by community workers (known as health surveillance assistants) are as reliable as arterial blood drawn by nurses, which is traditionally used to check viral load.
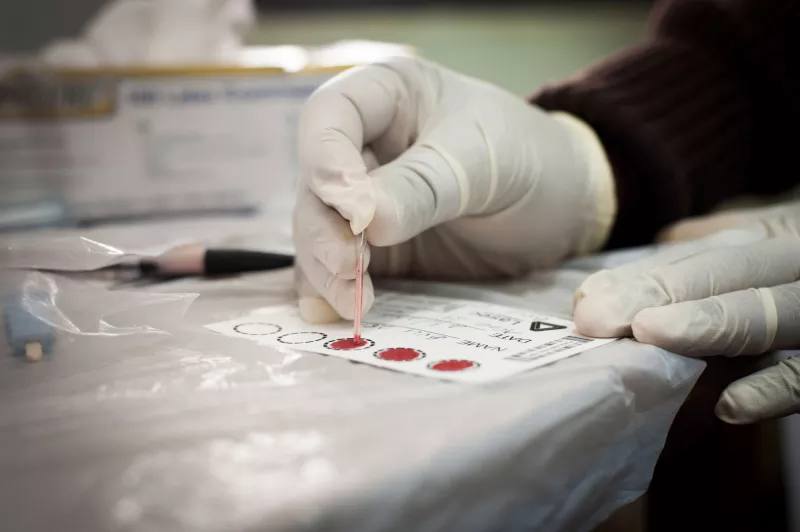
A health worker applies blood samples to DBS blotter paper. Moving basic medical tasks to less-skilled workers is called ‘task-shifting.” In this case, it expands the number of people able to gather samples for viral load tests, reducing dependence on Malawi’s scarce nurses and lab technicians. MSF continues to validate this approach in other countries as well.
DBS samples from the Bvumbwe Health Centre go to this lab at Thyolo District Hospital for viral load testing. MSF used a UNITAID grant to pilot a programme in Thyolo that pools DBS testing in local facilities. It avoids the need to ship samples to a distant central lab, which can mean waits of weeks or months for the results to come back.
Staff at the Thyolo District Hospital viral load laboratory, which can process 160 DBS samples. Results are sent to health workers by SMS for quick delivery. Decentralizing the testing process, pooling processing in local facilities and using blood spot testing all make HIV care faster and easier.
A support group for people living with HIV meets in the remote village of Chidothe,Thyolo District. “Before we started in 2003,” one member said, “people were very worried and there were many AIDS deaths in the community. We decided that if we came together, we could support each other.”
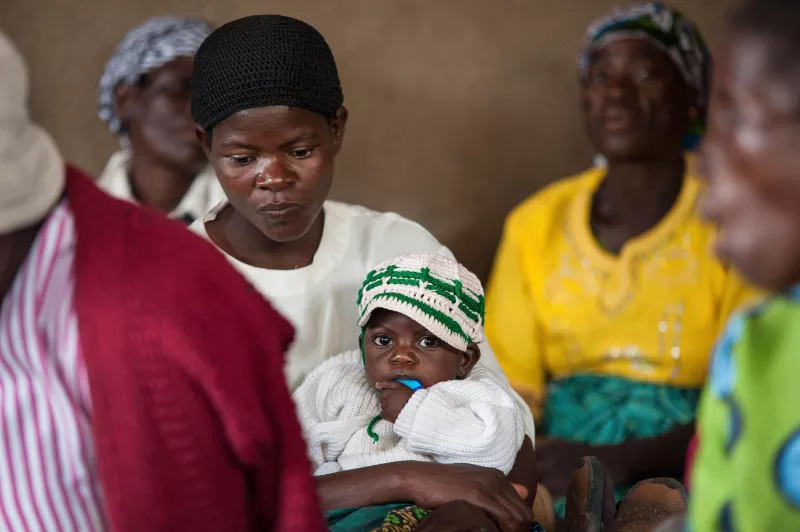
A woman and child at the support group meeting in Chidothe. Members take turns on a rotating basis to collect ARVs every month from a clinic five miles away, using a model piloted by MSF in Mozambique. When a leader asked how many in the group had been tested recently for viral load, nearly everyone raised their hands.
A waiting area at the Namitambo Health Centre, about 40km from the Thyolo District Hospital. Here, new point-of-care machines speed up processing for CD4 and viral load tests for people living with HIV. The machines allow clinicians to offer them same-day testing, sparing them a return trip to the clinic for results.
A lab worker at the Namitambo Health Centre uses a SAMBA machine to process viral load tests. This point-of-care machine generates results within a day, eliminates cold storage for processing materials and includes a back-up battery for the power cuts common in many developing countries.
Mercy, a mother living with HIV, walked 7 km to the Namitambo Health Centre for ARVs and her first viral load test. Health workers were concerned that she might not be taking her HIV medicines on schedule. If her test showed a high viral load, they planned to counsel her for three months on finding better ways to take her medicines on time.
All photographs by Giulio Donini