Qamar Ismail Yussuf, 22
Qamar’s journey into and out of Dadaab refugee camp in Kenya paints a picture of the journey that many Somali refugees have to take in the face of insecurity to pursue healthcare services. She first came to Dagahaley in 2009 with her mother and seven siblings, mainly to seek education and health services in the camp. “UNHCR refused to register us as refugees, so life in the camp became a little challenging, though it was a lot safer than in Somalia,” she says.
Qamar’s father had stayed in Somalia to look after his business, but in 2011 he fell sick and Qamar’s mother returned to look after him, taking five of her children with her, including Qamar.
Back in Somalia, Qamar started feeling unusually thirsty, as well as feverish and nauseous. “I would feel thirsty a lot and go to the toilet frequently,” she says. “I’d have high fevers and feel nauseous. We went to the local pharmacy and they gave me some intravenous fluids, but nothing changed. I would faint a lot and my family started saying I was possessed. Some of my relatives asked that I be brought to Dagahaley, where I was diagnosed with diabetes.”
Qamar was unconscious when she was brought to MSF’s hospital in Dagahaley in 2017. “I wasn’t even aware that we were here; I don’t know how we left Somalia,” she says. “A random blood sugar test was done and it turned 27 [mmol/L], from what I was told.”
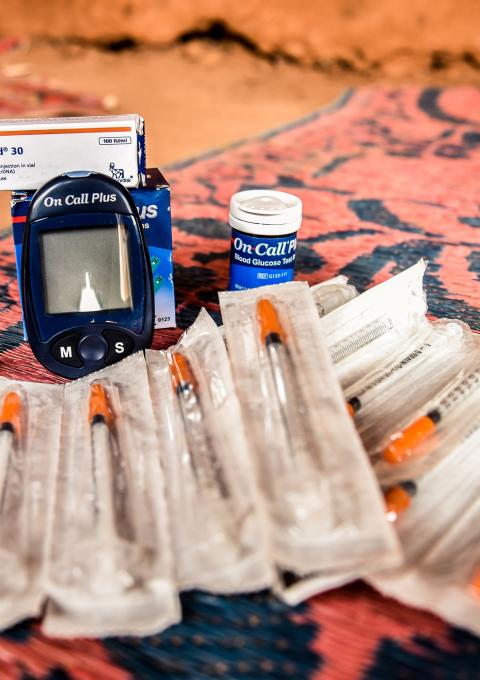
Qamar was admitted to MSF’s hospital for seven days while her blood sugar levels were monitored. “I felt huge relief when I was put on treatment,” she says. “After being discharged, I had to go to the emergency room every morning and evening to get insulin injections. It didn’t take long before we were trained and given a portable cooling box. It saved me a lot of time. Going to the ER every morning and evening, leaving my young children at home, was difficult. Now I am okay and nobody even knows that I have diabetes.”
Qamar says she has not faced any stigma since she started taking insulin, in contrast to the stigma she faced before being diagnosed with diabetes. “After I got this, it’s like I gained independence,” she says. “I can inject any time I feel like my sugars are high. Many people are injecting, and it’s something that people have come to understand. I carry my syringes and portable cool box whenever I go visiting my friends or relatives. I never leave them behind. There was this time I went home to Dhobley and Kismayu and I carried it. My relatives there were so fascinated to see me inject myself. They’d ask: ‘How do you inject yourself? Can you do it now so that we can see?’” she laughs.
Qamar says that MSF provides all the supplies she needs, including insulin and syringes. She has follow-up visits at the hospital every 14 days, when she collects more supplies.
Despite being on insulin for more than two years, Qamar says that pricking her finger to test her blood sugar levels is what she dreads most. “Pricking the finger every time is painful and injecting can lead to soreness,” she says. “But it never stops me from carrying out my daily activities. Every morning I check my fasting blood sugar before I eat or inject insulin and my random blood sugar. I can read and understand the glucometer well and know how much insulin to inject. I am prepared for the injections, so they never bother me. I don’t experience hypoglycaemia much, but if I don’t eat well and when I’m told to eat, then the sugar gets low.”
Qamar’s biggest concern is the lack of consideration she receives at the food distribution centres. “There is no special consideration whatsoever, whether you’re sick or not,” she says. “We queue there and, when I feel dizzy, I just sit down.”
“I really appreciate the services offered by MSF,” says Qamar. “The doctors are very professional and supportive. Only we know what it feels like to have diabetes and having the right diagnostics and treatment kits provides a huge relief.”
Fatuma Bare Hussein, 27
Fatuma is a mother of two vibrant young boys: four-year-old Abdirahman Ali Diyat, and two-year-old Abdullahi Ali Diyat. What stands out about her story is that she is fully healthy, but her two little boys both live with diabetes.
Abdirahman – Abdi, as they call him – was diagnosed with diabetes when he was nine months old. “He used to pass urine a lot and would look weak most of the time,” says Fatuma. “I took him to the nearby health post, where we were given some syrup to give him. But when he started losing weight, I took him back to the health post. They conducted a random blood sugar test and found that his blood glucose was too high. They asked if anyone in my family had diabetes, but there’s none that I know of. I thought only old people got diabetes, not children this young.”
When her second son was born, Fatuma recognised the signs. “For the younger one, I also saw similar symptoms,” she remembers. “I couldn’t believe it. How could it be? When Abdi was diagnosed, I felt stressed, knowing he’d have to take insulin for the rest of his life. When this little one was also diagnosed, I almost gave up. I cried.”
Fatuma says her life has not been normal since Abdi was diagnosed with diabetes, and it got even more abnormal when Abdullahi had the same diagnosis.
“These are kids – they don’t know the seriousness of their condition,” she says. “Sometimes when it’s time to inject them, they run and I have to chase after them. Then they’re difficult to restrain when they see the syringe. At times you find some insulin remains in the syringe and you have to inject it into them. You know, with babies it’s very difficult to know how they are feeling – they may not be able to express the discomfort they are in. They used to cry a lot. Sometimes the sugar is low, sometimes it’s high – it’s difficult to know. The youngest one is the most difficult to handle. The four-year-old started [insulin injections] a while back and is already used to it; he thinks it’s a daily routine. My biggest fear is controlling what the kids eat when they are playing out there. They may eat sweets or other things they’re not supposed to eat; it stresses me at times.”
Fatuma says she was well trained by MSF prior to being given her own portable cooling box and insulin for her children. She understands what each reading means and what to do in each instance.
Ali Bishar Adan, in charge of MSF’s home-based insulin management programme, says Abdi was the first patient to be enrolled into the programme. “He is our patient number 001 under the programme and the mother has been one of the best,” he says.
Fatuma says the only challenge associated with the cooling box is that rats sometimes chew it, and scorpions and other small insects crawl inside to keep cool in Dadaab’s hot climate. But she cleans the box frequently and has learnt to hang it in a place where the insects cannot easily reach it.
For Fatuma, the biggest challenge is getting hold of enough food so that she can feed the children to coincide with their injections. “I inject each of them twice a day: in the morning and in the evening,” she says. “With every injection, the children need to eat. If we were to inject more frequently, where would I get the food to give them? I don’t have a job, and the food ration we are given by WFP is hardly enough for seven days.”
The younger boy experiences hypoglycaemia at least twice a week and sometimes more frequently, especially at night. “He does not eat well,” says Fatuma. “I try to force him to eat but he will not eat much. So I usually keep some food in a cooking pot or some milk to give him at night. I used to give them sweets and biscuits, but their teeth started decaying, so I stopped.”
Mohamed Hussein Bule, 27
Mohamed is well dressed and speaks fluent English. He is a teacher in a primary school in Dagahaley, where he teaches science to the two highest classes.
Mohamed came to Dadaab in 1992 with his mother after fleeing violence in Somalia. He went through his schooling in the camp and is now pursuing a bachelor’s degree in education at a local university, sponsored by one of the agencies in the camps.
Mohamed got married eight years ago, when he was 15 and his wife was 18. His wife helped care for his sick mother while he focused on his studies.
“My mother was very sick and had no one to take care of her,” he says. “I needed to concentrate on my studies to have a better future and my sister was too young at that time. My wife cared for my mum very well.” Mohamed and his wife now have four children, all of whom were born in Dadaab.
Mohamed was keen on football but had to stop playing when his health suddenly deteriorated. “I used to play soccer, but I stopped in 2014 as I would get exhausted,” he says. “I started passing urine frequently and lost weight, going from 68 kg to 35 kg.”
While visiting an uncle in Nairobi in 2016, he went to a health facility where his blood sugar was tested and found to be high. He was provided with insulin, paid for by his uncle, which he took three times a day. One month later, he returned to Dadaab and came to MSF’s Dagahaley hospital.
“I went to the hospital and my treatment was changed,” he says. “Said [the former supervisor of MSF’s home-based insulin management programme] was good. He trained me a lot to be how I am today. I don’t even feel like I am diabetic. He taught me how to inject, how to understand hyper- and hypoglycaemia. I always wish him a successful life in future.”
Mohamed injects himself with insulin twice a day and has a follow-up visit at the hospital every three weeks. “The doctor here plans the schedules for us,” he says. “Myself I go for review every 21 days, when they also replenish our supplies. The insulin in the bottle is usually enough for 21 days.”
Mohamed says the portable cooling box is even better than the refrigerator he used before. “When you use a refrigerator, sometimes it gets too cold, so that when you inject it makes you cringe a bit,” he says. “I carry mine even to class and it does not bother anyone. People know that diabetes is not contagious, and if something can’t be transmitted, then people don’t get too concerned.”
The main challenge of the regimen, says Mohamed, is that he can’t eat for at least 30 minutes after taking insulin.
Mohamed has no problems using the glucometer. “Interpreting glucometer results is quite easy,” he says. “It works very fast and makes a beep when it’s ready. I know what range is supposed to be high or low.” Occasionally he experiences hypoglycaemia, or low blood sugar, but he has developed strategies to deal with it. “The last time I experienced it was during Ramadan, when we usually fast,” he says. “It also happens when I travel or when I walk for too long. The best way is to carry sweets in the pocket, but only eat them when you feel hypoglycaemia kicking in.”
Being a refugee presents many challenges, says Mohamed, but life in Dadaab has improved in some ways since he was a child. “When you’re a refugee, you can’t get everything you need,” he says. “When I was a child, life was difficult, but the camp has really developed over time, even the market. Travel is also difficult as movement is restricted. I find it quite difficult when I have to go to the university for my classes.”