Out of Step: TB policies in 29 countries, 3rd Ed.

Although it can be prevented and successfully treated, tuberculosis (TB) is the world’s deadliest infectious disease: in 2015, 1.8 million people died from it.1
While there have been substantial and important innovations in the fight against TB, including faster, more accurate diagnostic tests and the first new medicines in nearly 50 years, deadly gaps remain in implementing and providing access to these advances. Outdated policies, practices and tools for diagnosing, as well as conservatism and inaction in registering and using new TB medicines, are key barriers to turning around the TB epidemic. Adopting and implementing internationally recognised TB policies and guidelines from the World Health Organization (WHO) is fundamental to ending TB by 2030. But the Out of Step 2017 report reveals that many countries still lag behind in ensuring full implementation of the WHO guidelines and policies that are proven to reduce TB incidence and death.
About Out of Step 2017
Out of Step 2017 includes the results of a 29-country survey on national TB policies and practices. The report was created to identify gaps in implementation and monitor progress towards ending TB. While countries have made progress since the Out of Step 2015 report, much more work needs to be done to make sure that these policies are fully implemented across all communities, so that they will make a real difference to people affected by TB.
Additional publications in the Out of Step report series are available here.
Learn more about MSF’s work to improve access to lifesaving TB treatment.
About Out of Step in EECA
Out of Step in EECA is a regional adaptation the Out of Step 2017 report that focuses on TB diagnosis and treatment challenges in Eastern Europe and Central Asia (EECA). An epidemic of drug-resistant TB (DR-TB) is on the rise in EECA, where nearly half of all TB cases are multidrug-resistant and the number of people with DR-TB is increasing by more than 20% each year.
Read and download:
Out of Step 2017 (English): Fact sheet
Out of Step in EECA (English): Fact sheet
Out of Step in EECA (Russian): Fact sheet
Countdown to 2030
In 2015, world leaders endorsed the United Nations Sustainable Development Goals, which include an ambitious but achievable target to end the TB epidemic by 2030.2 The WHO’s End TB Strategy, which was approved by the World Health Assembly in 2014, calls for bold policies and supportive systems at the national level, and reductions in TB incidence (by 80% from 2015) and TB deaths (by 90% from 2015) by 2030.2
The Stop TB Partnership’s Global Plan to End TB 2016-2020 sets out the actions and resources needed by 2020 if the world is to end the epidemic by 20303; it challenges countries to reach the 90-(90)-90 targets: to have 90% of all people with TB diagnosed and successfully treated, including 90% of vulnerable populations.
Diagnosis
Diagnosing TB quickly and accurately, so that people receive appropriate treatment, is an imperative first step. While many countries have adopted WHO guidelines and policies for diagnosis, the glacial pace of implementation is costing both lives and livelihoods. In 2015, more than 4 million people with TB went undiagnosed, and less than 25% of people estimated to have drug-resistant TB were diagnosed and treated.1
The first step to closing the deadly diagnostic gap is initial testing for all with Xpert MTB/RIF, a rapid molecular test that can diagnose TB and detect rifampicin resistance in 2 hours. For people with rifampicin-resistant (RR) TB, additional drug-sensitivity testing (DST) should be available so that they can be treated with medicines most likely to be effective. In the 29 countries surveyed, 52% (15) have adopted a policy of ‘Xpert for all’ and 47% (7/15) of them have widely implemented the test. Of all countries that provide initial testing with Xpert MTB/RIF only to high-risk groups (people living with HIV and people at risk for drug-resistant forms of TB), only 54% (15/28) have widely implemented it. Universal DST must be scaled up: 62% (18) of countries recommend it and 50% (9/18) of those have widely implemented it. With such a low proportion of countries having fully implemented recommended tests, the diagnostic gap remains massive; this deadly gap must be closed so that countries can reduce TB illness and death.
Models of care
Once a person with TB has been properly diagnosed and started on treatment, ongoing care must be patient-centred, and easily accessible to all who need it. It has been more than 50 years since WHO recognised that limited resources were best used for ambulatory TB care, instead of hospital beds. Decentralising TB treatment relieves the deadly bottleneck delaying treatment initiation, lowers the cost of treating TB and is preferred by patients. Community health workers can improve drug-resistant (DR) TB treatment adherence by providing education, support and counselling and they facilitate decentralisation of DR-TB treatment. Drug-sensitive (DS) TB treatment is started at the primary health care level in 83% (24) of countries (in some countries exceptions are made for people who are smear-negative and on a case by case basis), and 83% (20/24) of them have implemented the policy widely. Only 52% (15) of countries allow nurses and other health care workers to start adults on treatment for DS-TB. In 66% (19) of countries surveyed, treatment for DR-TB is initiated at the district level; but only 58% (11/19) of them have implemented the policy widely. Although hospitalisation should be reserved only for the sickest DR-TB patients, 34% (10) of countries still require it for nearly all patients. These results indicate that the decentralisation of patient-centred care must significantly accelerate if countries are to seriously improve treatment outcomes for people diagnosed with TB.
TB is the leading cause of death among HIV-positive people; HIV increases vulnerability to TB by up to 31-fold.4 In 2015, 400,000 HIV-positive people died of TB.1 Antiretroviral therapy (ART) lowers the risk for TB, and is recommended by WHO for all HIV-positive people.5 Yet, only 38% (11) of countries have adopted ‘HIV test-and-start’ policies, and only 73% (8/11) of them have implemented the policy widely. These findings illustrate that much more needs to be done to prevent people living with HIV from developing and dying from TB co-infection.
Treatment
Children are especially vulnerable to TB. In 2015, 1 million children fell ill with TB1, and approximately 169,000 children aged 0-14 died from it.1 The lack of child-friendly drug formulations has complicated paediatric TB treatment, but child- and caregiver-friendly paediatric fixed-dose combinations (FDCs) for DS-TB are now available and recommended by WHO. In 50% (14/28) of countries, the new paediatric FDCs for DS-TB are the standard of care, but only 29% (4/14) of them have widely implemented this policy. Children have long been neglected in TB care due to the difficulty of diagnosing and treating the disease. Nevertheless, governments must clearly do more to ensure the new paediatric formulations are reaching patients. Treatment for DR-TB can be shortened to 9 months in certain circumstances; for people who are eligible, shorter treatment is equally effective and spares them from months of terrible side effects, and saves money. But only 45% (13) of countries recommend it, and only 69% (9/13) of them have implemented it, but not widely. Bedaquiline and delamanid, newer TB medicines recommended for people with few or no TB treatment options, are included in 79% (23) and 62% (18) of national guidelines, respectively. Globally, however, only about 5% of people with DR-TB have access to these life-saving medicines. Out of Step reveals that countries are too conservative in implementing new treatment regimens that could significantly improve cure rates for DR-TB, and help curb the spread of drug-resistant strains.
Regulatory environment for TB medicines
Access to new treatments must be accelerated. This requires that governments take bold steps in how drugs are regulated and made available in their countries. Only 75% (21/28) of countries have accelerated registration mechanisms in place, while 89% (25/28) of countries allow access to unregistered TB medicines through compassionate use programmes, import waivers, or by other means. Furthermore, 41% (12) are enrolled in the WHO Collaborative Registration Procedure, which accelerates approval of and access to originator and generic medicines, including TB medicines, for public health needs in developing countries. None of the 29 countries surveyed list all of the anti-TB medicines recommended by WHO for the treatment of DR-TB in their national Essential Medicines List (EML) in the TB medicines section and only 25% (7/28) include bedaquiline or delamanid in their national EML.
Prevention
TB can be prevented. Preventive therapy can stop people with latent TB infection (LTBI) from developing active TB disease. But access is not universal; while all of the countries provide it to the most vulnerable groups (child contacts and HIV-positive people), 31% (9) of these countries have not implemented it widely. Only 14% (4) of countries provide preventive therapy to other high-risk groups, and only 14% (4) of countries also provide it to adult contacts. Countries must pay more attention to TB prevention if they are to make serious inroads in stopping the spread of this debilitating and deadly disease.
Conclusion
The Out of Step findings clearly show that governments must re-commit to fighting and winning the battle against TB, with urgency. Global health actors, governments and donors urgently need to step up to stop the world’s poorest and most vulnerable people from needlessly falling ill, suffering and dying from TB. Although we have modern tools for fighting this ancient disease, we aren’t using them enough - especially in the places where they are needed the most. We are still out of step in preventing and diagnosing TB, providing patient-centred care, and accelerating research into, registration and delivery of new, life-saving medicines. We urgently need political will and adequate resources to fight TB; only a third of the annual funding needed to meet the 2030 targets is being provided. Without funding, we will not be able to fully roll out the policies, practices and tools that spare people with TB from avoidable suffering and death.
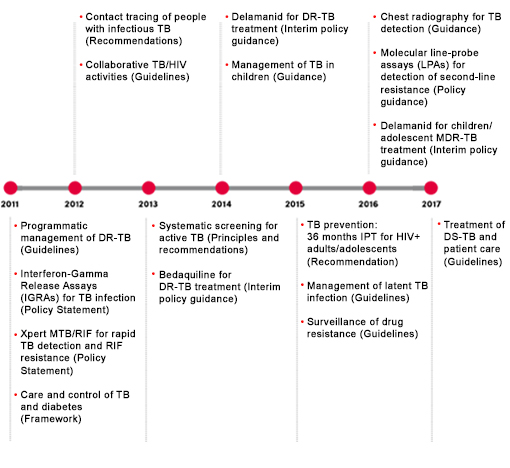
Timeline of key WHO policies and guidelines (2011-2017)
References:
1. WHO. Global tuberculosis report 2016. [Online]. 2016 [Cited 2016 Dec 12]. Available from: http://www.who.int/tb/publications/global_report/en/
2. WHO. Implementing the End TB Strategy: the essentials. [Online]. 2015 [Cited 2017 May 31]. Available from: http://www.who.int/tb/publications/2015/end_tb_essential.pdf
3. Stop TB Partnership. The paradigm shift 2016–2020: global plan to end TB. [Online]. 2015 [Cited 2017 May 17]. Available from: http://www.stoptb.org/assets/documents/global/plan/GlobalPlanToEndTB_TheParadigmShift_2016-2020_StopTBPartnership.pdf
4. WHO. 10 facts on tuberculosis. [Online]. 2017 Mar [Cited 2017 Mar 29]. Available from: http://www.who.int/features/factfiles/tuberculosis/en/
5. WHO. Guideline on when to start antiretroviral therapy and on pre-exposure prophylaxis for HIV. [Online]. 2015 Sept [Cited 2017 Mar 27]. Available from: http://apps.who.int/iris/bitstream/10665/186275/1/9789241509565_eng.pdf?ua=1