10 June 2021
Dr Christos Christou, MSF’s International President:
“Ongoing widespread transmission of the virus in regions with poor access to treatment, vaccines, testing and other protections means COVID-19 continues to claim thousands of lives each day and viral variants develop more easily, pushing health systems in many countries where MSF works to the brink of collapse. It’s precisely the actions of the G7 governments, among others, that have led to the grave global inequities we see in access to COVID-19 medical tools now, despite several of these leaders having stated early on that such tools should be treated as ‘global public goods’.
“While several G7 countries are well on their way to getting back to ‘normal,’ having pursued herd immunity strategies before sharing doses with others, most low- and middle-income countries have been left empty-handed as they face additional deadly waves of disease. G7 countries, which have ordered many more vaccines than they need, should immediately share as many doses as possible with low- and middle-income countries. Every day that passes is another missed opportunity to protect millions of people globally from this killer disease.
“With vaccine manufacturers shifting their responsibility of legal liabilities to countries in the event of serious adverse events, governments and humanitarian organisations have been put in a precarious situation by this unacceptable transfer of risk. The onus of such responsibility must not be pushed on to organisations that are willing to vaccinate and should not become a barrier for people who need them.
“As vaccination has started around the world, albeit mainly in developed countries, there is nonetheless a wealth of data that should be used to revisit the issue of liability and indemnification. This is not about a simple business transaction but about saving lives and preserving health. It is time for manufacturers to resume their responsibility for their own products, and for governments, including the G7, to exercise their authority in making this a reality.
“During the pandemic, we’ve repeatedly seen how control of global production and supply of lifesaving medical tools based on intellectual property and technology ownership by a handful of multinational pharmaceutical corporations has created multiple obstacles for countries to secure reliable access. G7 leaders have so far not shown any willingness to break from the status quo and exert influence on pharmaceutical corporations for sharing the technology that was largely developed with public funding.
“G7 governments must urgently work with other governments to use all policy options available to facilitate and mandate transparent, unconditional, enforceable and full transfer of technologies of COVID-19 medical tools, particularly vaccines, by companies they host to manufacturers in all regions, and especially in low- and middle-income countries, in order to ensure access for everyone, everywhere. It’s time for change, not charity.
“It is regrettable that over half of the G7 leaders continue to ignore low- and middle-income countries’ demands to be self-reliant in the production and supply of medicines, vaccines and diagnostics needed to tackle the pandemic. Instead, they keep blocking critical decisions in multilateral fora to lift corporate monopolies in the pandemic to facilitate global production and diversification of supply, such as the proposed temporary COVID-19 intellectual property waiver at the World Trade Organization. G7 leaders must act in solidarity and support necessary measures to ensure that each country has sufficient tools to save as many lives as possible in this pandemic.”
Background:
G7 leaders are meeting to discuss pandemic response against the backdrop of over 3.7 million COVID-19 deaths and alarming and growing inequity around access to COVID-19 medical tools. These leaders have not taken steps to ensure that the scarce supply of COVID-19 medical tools is equitably shared based upon the public health criteria outlined by the World Health Organization, instead aiming to reach herd immunity for their own populations before even the most vulnerable people are vaccinated in low- and middle-income countries.
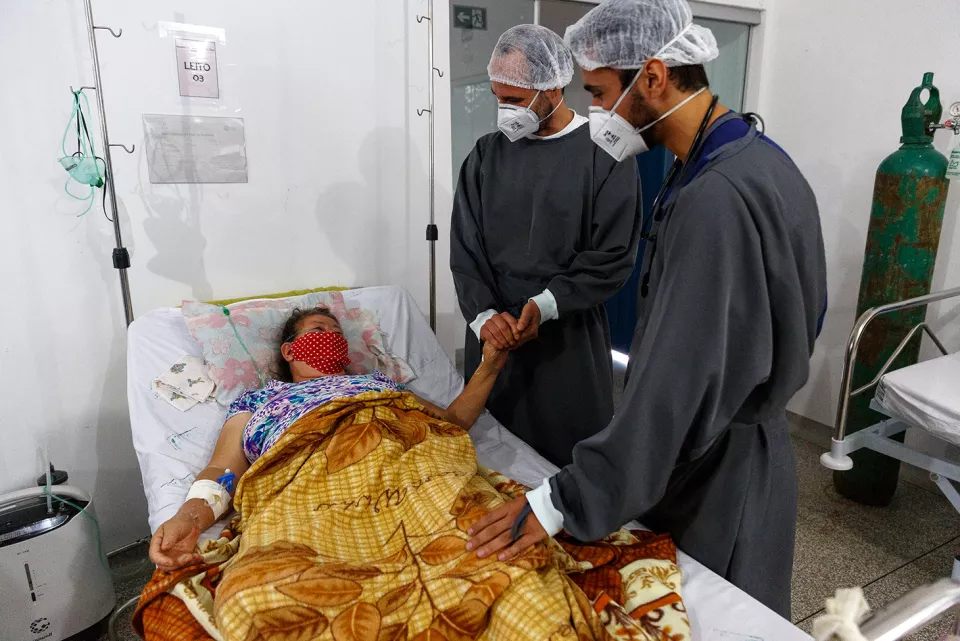
In the last few months, healthcare workers, including those from Médecins Sans Frontières/Doctors Without Borders (MSF), have struggled to provide care during multiple waves of the pandemic in countries such as Brazil, Peru and India. With their healthcare systems on the verge of collapsing due to emerging waves, it has been very challenging to provide any supportive therapies to critically ill COVID-19 patients in hospitals, as the oxygen concentrators, ventilators and medicines remain in short supply. As new and more transmissible variants of the virus continue to emerge and impact many countries, urgent measures should be taken by G7 governments to ensure that all COVID-19 medical tools are accessible and affordable for everyone.
A recent study shows that of the 1.77 billion doses of COVID-19 vaccines given globally, 28% have been in G7 countries themselves, while in contrast just 0.3% have been given in low-income countries. This despite the fact that the G7 countries together have around the same total population as all low-income countries combined, meaning that for every person vaccinated in a low-income country, 100 people have been vaccinated in G7 countries. G7 countries must take immediate action to allocate COVID-19 vaccine doses to the COVAX Facility. This should be done in two ways: first, by G7 countries refraining from drawing on COVAX supply themselves, and second, by G7 countries that have vaccinated over 20% of their population immediately allocating their remaining vaccine doses to COVAX.
There has been unprecedented public funding for COVID-19 research and development (R&D), manufacturing, and advance purchase of vaccines and treatments: one analysis finds that governments have spent over US$113 billion, with additional pledges ongoing. However, there is very little transparency and accountability regarding how these funds are being used. The critical issues of where production should happen, who gets the products and at what prices remain largely controlled by pharmaceutical corporations. Presently, confidential and restrictive bilateral licensing and technology transfer agreements signed between companies lack adequate public oversight and regulation.
Global mechanisms that have been set up to increase equitable access to COVID-19 medical products, such as the Access to COVID-19 Tools Accelerator (ACT-A), which comprises the COVAX Facility, have so far failed to ensure that transparency is a core principle and deliverable within their functioning, accountability and governance. Critical information, including prices, manufacturing capacity, delivery schedule and agreements with pharmaceutical corporations are not made public, making policy analysis of the real impact of ACT-A (and COVAX) in achieving equitable access very difficult.
Governments and global health institutions, such as those involved in ACT-A, should attach conditions to all funding, requiring full disclosure of R&D and manufacturing costs, prices, intellectual property (IP), licensing agreements and clinical trial data. All agreements and contracts with industry must also be made public in full. Any R&D funding should be conditional on granting-back legal ownership of the technology to the government, and sharing know-how, technologies and IP on a non-exclusive basis with global coverage.
As countries have started to procure vaccines, agreements with the manufacturers include special clauses on liability and indemnification. Under normal conditions, manufacturers accept full liability for vaccines and medical products produced by them and are insured against any potential losses. However, in this pandemic, pharmaceutical corporations have sought indemnification in the event there are claims of serious adverse events and have shifted that responsibility to countries, making governments liable. While there is a compensation mechanism put in place for some low- and middle-income countries receiving vaccines from the COVAX Facility, such measures are not necessarily applicable to many other self-financing countries. Furthermore, this burden is now being extended to humanitarian organisations seeking to vaccinate marginalised populations such as refugees, displaced persons, populations in non-government-controlled areas, etc. For organisations working on the frontline, it is a dangerous precedent and risks eroding the trust of communities, which is critical in ensuring safe access and delivery of health services to vulnerable populations.