Paris, 27 July 2017 — Zimbabwean MSF nurse and researcher Chenai Mathabire has won an HIV/TB Research Prize at this year’s International Aids Society Conference on HIV Science (IAS2017). Through a study conducted in Malawi and Mozambique, Chenai has provided strong evidence that an easy-to-use point-of-care TB LAM test, which quickly diagnoses tuberculosis (TB) in severely ill HIV patients, is feasible to use in real-life clinics with high numbers of HIV-TB patients.
TB is the biggest killer of people living with advanced HIV, with over 400,000 patients dying each year from the disease. People with advanced HIV, also known as Acquired Immune Deficiency Syndrome (AIDS) have very weakened immune systems, leaving them susceptible to common infections, which can quickly become deadly.
Successfully treating ill AIDS patients involves rapidly assessing the strength of their immune systems and putting them on the right treatment straight away, whether they have TB or another disease deadly to HIV patients, cryptococcal meningitis.
However, in poorer countries, limited laboratory and X-ray facilities, and the time spent waiting on results can mean long and often deadly delays for sick patients arriving at clinics or hospitals. At the same time, people with late-stage HIV often can’t produce enough sputum for more common TB sputum tests so common tests such as sputum microscopy cannot be done. X-rays are also less useful to detect TB in people with advanced HIV.
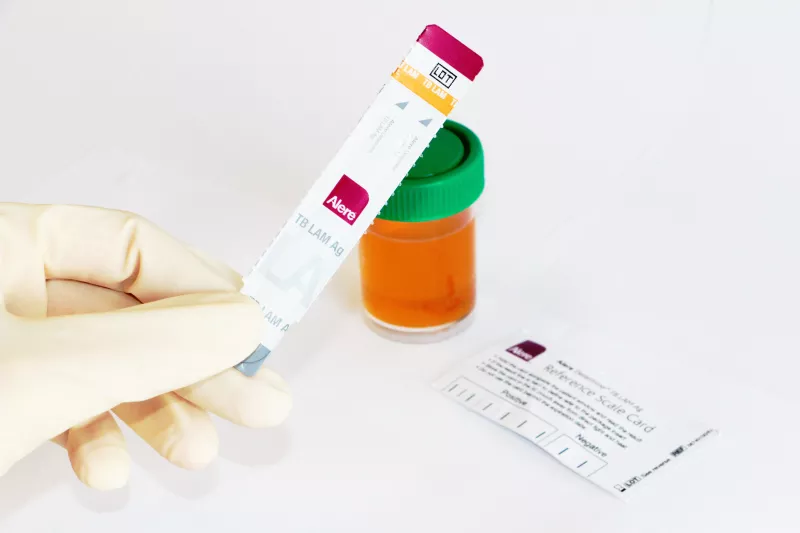
At $3 per test, the TB LAM test offers a quick, simple and cost-effective alternative that gives on-the-spot results in 30 minutes. Yet despite being available since 2010, only 140,000 TB LAM tests are used each year. “In Malawi, some HIV patients with suspected TB were waiting for months for laboratory or X-ray results to come back. Clinicians don’t like to start patients on treatment based only on clinical signs and symptoms, they prefer to have a diagnostic test result,” says Chenai, who was responsible for implementing and supervising the study. “The TB LAM test helped them make that decision, and they felt better about starting HIV patients on TB treatment. It doesn’t replace existing tests, but adding this test helps us identify more TB cases and can improve the patients’ chances of survival.”
The test uses the HIV patient’s urine to detect LAM (Lipoarabinomanan), a protein created when TB bacteria cells break down. The lower the patients’ immunity, which is measured by numbers of CD4 T-cells, the more LAM appears in the urine and the more sensitive the test becomes. This is why the test is recommended for use in patients with CD4 cells below 100. The MSF study found the test was well accepted by staff, easy to use, and led to better, faster results than sputum or X-ray tests. Nearly 99% of TB LAM test patients received a timely result, versus 70% with sputum and 35% with X-rays.
Currently, the main barrier to wider use of the TB LAM test by national governments is that it isn’t included in country guidelines and national TB programmes are not actively pushing it. Use of the TB LAM test has been recommended by the new WHO guidelines for advanced HIV for use in severely ill patients in hospitals but not yet in primary care, given the test’s decreased accuracy in patients with stronger immune responses.
MSF will use the study to advocate for health ministries in countries with high HIV TB burdens to use the TB LAM test in primary care and hospital centres, as well as include TB LAM within a diagnostic package for patients with advanced HIV. This would include point-of-care tests for CD4 (to allow rapid bed-side assessment of immune strength), cryptococcal meningitis and TB to help quick diagnosis and, most importantly, improve patients’ chances of survival.
MSF currently uses TB LAM as part of a diagnostic package in HIV projects in Democratic Republic of Congo (DRC), Guinea, Kenya, Malawi, Mozambique, Niger, Uganda, and Zimbabwe. MSF currently supports over 230,000 people living with HIV on antiretrovirals in 19 countries, with a focus on free quality care, and provides free hospital-based care for people living with advanced HIV in DRC, Kenya Guinea, and Malawi.