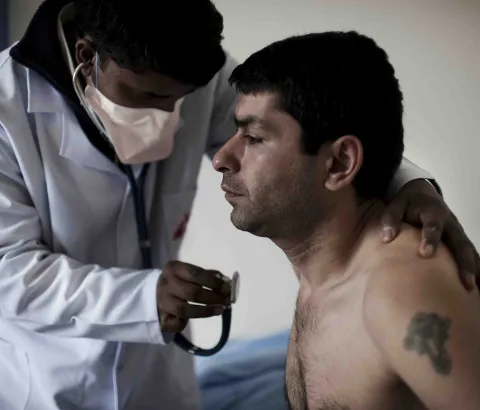
The Head of the Paediatrics Department at Gujranwala Teaching Hospital in Pakistan’s Punjab province, Dr Saima Umar, shares her experience of how WHO recommended TB Treatment Decision Algorithms are helping diagnose children more effectively and the challenges doctors faced before their introduction.
Dr Umar has been providing paediatric services for the past nine years. Over the last year, she has also been working with Medecins Sans Frontieres (MSF), which supports the Programmatic Management of Drug-Resistant Tuberculosis (PMDT) site at the same facility. Since July 2024, MSF has also been implementing the TACTiC initiative at the project.
We asked Dr Umar to share her experiences.
Before using TB treatment decision algorithms, what were the biggest challenges in diagnosing TB in children?
There have always been diagnostic challenges when it comes to TB in children. Even if we suspect clinically that a child has TB, the diagnostic process becomes difficult because children often cannot produce sputum samples, and the yield from sputum tests is usually very low.
Before the WHO TB treatment decision algorithm, we used the Pakistan Paediatric Association (PPA) scoring system to diagnose TB in children, but even while applying it, we often had doubts about whether we should start TB treatment.
TB treatment is not short; it requires proper counselling and continues for several months. Because of this, we always had to think carefully before initiating treatment, considering possible side effects. We were also concerned about whether we might be overtreating or undertreating the patient.
How have the WHO TB treatment decision algorithms changed your confidence in initiating treatment for children?
With the WHO TB treatment decision algorithm, it has become much easier for us. It has made diagnosing patients simpler and increased our confidence in starting treatment. Earlier, we were often uncertain if we did not start treatment, the disease might progress; but if we started treatment without a clear diagnosis, there could be unnecessary side effects.
The algorithm has really helped because it is evidence-based, and it gives us greater confidence in our decisions.
Previously, there were patients who fell into a borderline category. We suspected that the child had TB, but the tests did not show positive results. Since obtaining proper test samples from children is very difficult and we often lacked sputum evidence, it was challenging to make a firm decision. This algorithm has helped us a lot in such cases.
It has also significantly reduced delays in starting treatment in children. TB can spread quickly in children and can lead to serious infections. Any delay in starting treatment can worsen their condition.
Children with TB are often the first to be left behind. Why must this change?
In Pakistan, the young population is very large. Children are highly vulnerable to infection from adults and can become affected very quickly. Therefore, it is very important to prioritize children. Working for children means working for our future.
TB in children should be understood as a silent emergency. There needs to be more active focus and effort in this area so that our next generation can remain healthy and productive.