MSF teams are racing to respond to the COVID-19 pandemic in over 70 countries, including opening projects in new countries as they become pandemic hotspots.
Our COVID-19 response focuses on three main priorities:
• supporting authorities to provide care for COVID-19 patients;
• protecting people who are vulnerable and at risk;
• and keeping essential medical services running.
Across our projects, MSF teams have been improving infection prevention and control measures to protect patients and staff, and prevent further spread of the new coronavirus. It is absolutely crucial to prevent health facilities from amplifying the pandemic or being forced to close their doors.
Health systems worldwide are urgently in need of personal protective equipment – which face shortages of crucial items such as masks and aprons – so that essential medical services can stay open.
Having access to protective equipment, to COVID-19 tests, to oxygen and to drugs for supportive care, becomes more and more urgent as COVID-19 spreads in countries with little access to these tools.
Protecting people living in precarious conditions
Of particular concern is how coronavirus COVID-19 might affect people in precarious environments, such as the homeless, refugees living in camps in Greece or Bangladesh, or conflict-affected populations in Yemen or Syria. These people live under harsh, often unhygienic and overcrowded conditions, where their access to healthcare is already compromised.
How can we ask people to protect themselves when they don’t have easy access to water? Or to stay at home and self-isolate if they rely on daily jobs to make ends meet, or share a room with 10 other people? Nonetheless, it is very important to inform people of protective measures (such as washing their hands often) and help ensure they have the means to protect themselves (including self-isolation in case of contact with a person infected with COVID-19).
If COVID-19 starts to be transmitted in fragile settings like these, it will be practically impossible to contain. Basic health screening and, ideally, decentralised testing for high-risk settings such as refugee camps (Cox’s Bazaar in Bangladesh or on the Greek islands, for example) or high-density slum dwellings (Kibera in Kenya or Khayelitsha) needs to be implemented immediately.
Keeping healthcare workers safe
Protecting healthcare workers from contracting the virus is paramount for ensuring the continuity of care for general and COVID-19-related health needs. However, global shortages of personal protective equipment (PPE) pose a great threat. Healthcare workers must have access to the equipment they need to do their jobs safely and effectively.
Challenges in ensuring continuous care in MSF projects
We want to ensure continuous care for all patients where we work today and prepare our medical teams to manage potential cases of COVID-19. Protecting patients and healthcare workers is essential, so our medical teams are also preparing for potential cases of coronavirus disease COVID-19 in our projects. This means ensuring infection prevention and control measures are in place, including setting up screening at triage zones, creating isolation areas, and providing health education.
Our projects are still able to continue medical activities, but ascertaining future supplies of certain key items, such as surgical masks, swabs, gloves and chemicals for diagnosis of COVID-19, is a concern. There is also a risk of supply shortages for other diseases due to a lack of production of generic drugs and difficulties to import essential drugs (such as antibiotics, antimalarial and antiretroviral drugs), caused by community lockdowns, reduced production of active pharmaceutical ingredients, and reduction in export movements.
We face additional challenges because travel restrictions linked to COVID-19 are limiting our ability to move staff between different countries. We are trying to find ways to manage this, to avoid heavily impacting projects needing specialist profiles, such as surgeons. However, international staff represent just eight per cent of our total global workforce, so most MSF projects are run by locally hired team members.
Ensuring access to medicines, vaccines, and diagnostics
MSF seeks to ensure that the medical tools urgently needed to respond to COVID-19 are accessible, affordable, and available to all countries equally. All concerned stakeholders—including governments, pharmaceutical corporations, philanthropic organisations and research organisations developing treatments, diagnostics, and vaccines—should take the necessary measures to:
- Ensure the rapid and ample production of medical tools, once approved, and allocate supply based on equity and need.
Corporations should commit now to sharing data, providing technical know-how to generic manufacturers to facilitate production as needed, and not enforcing intellectual property. Governments should work in solidarity to meet not only their domestic needs but also to support other countries to get access to medicines, diagnostics, and vaccines.
- Prevent patents and monopolies from limiting production and affordable access.
MSF calls for no patents or profiteering on drugs, tests, or vaccines used for the COVID-19 pandemic, and for governments to prepare to suspend and override patents and take other measures including prices controls, to ensure availability and affordability to save more lives.
- Prioritise the availability of the medical tools for protection and treatment of frontline healthcare workers.
This includes any treatments for COVID-19, including drugs to prevent infection (pre-exposure and/or post-exposure prophylaxis) for frontline healthcare workers, especially in developing countries.
- Improve transparency and coordination among governments and other buyers to monitor and mitigate supply chain risks.
Rationing of medical tools because of high prices and insufficient supply will only serve to prolong this pandemic. An evidence-based approach should be put in place to continuously monitor the risk of any supply chain vulnerabilities at the national and global level – and their impact on access to all essential medicines, vaccines and diagnostics – and to adopt measures to mitigate supply chain risks through international collaboration.
MSF response to COVID-19
It is clear that healthcare workers need support and patients need care. Given the size of this pandemic, MSF’s ability to respond on the scale required will be limited. Find out how we are responding to the pandemic around the world.
Highlights of our COVID-19 response activities can be found in the interactive map below; click on a country to read brief information.
(The map and links below are not exhaustive of all of our COVID-19 response)
Visit the following links for details on country operations:
🇮🇷 Iran 🇸🇾 Syria 🇬🇷 Greece 🇮🇹 Italy 🇧🇪 Belgium 🇪🇸 Spain 🇫🇷 France 🇮🇶 Iraq 🇲🇱 Mali 🇳🇬 Nigeria 🇸🇩 Sudan 🇾🇪 Yemen 🇧🇷 Brazil 🇲🇽 Mexico 🇺🇸 USA 🇵🇰 Pakistan 🇰🇭 Cambodia 🇵🇬 Papua New Guinea
How can I prevent myself from being infected with COVID-19?
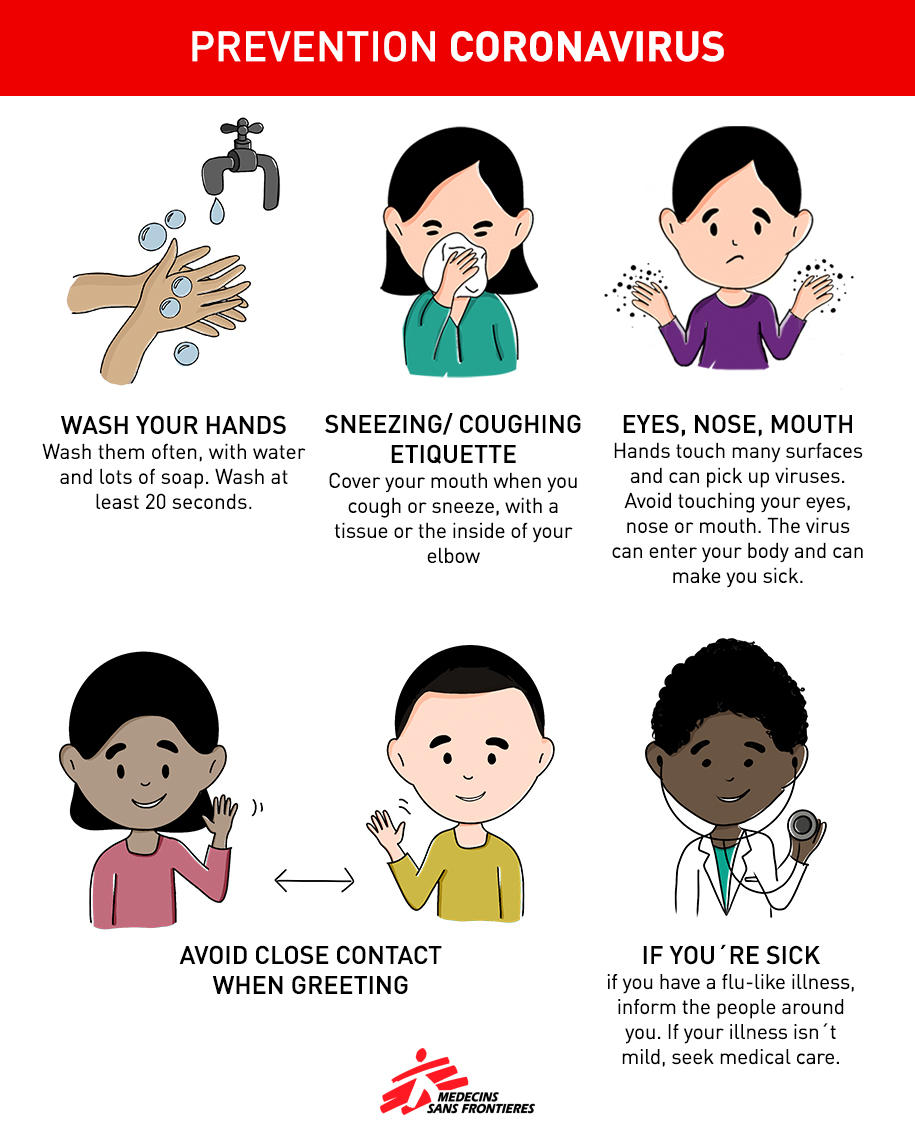
It is important to protect yourself and others. As with other coronaviruses, droplet infection seems to be the main mode of transmission. The virus enters the human body through the mouth or nose. This can happen by breathing in infected droplets, or by touching with your hands a surface on which droplets have landed, and then touching your eyes, nose, or mouth later. Simple infection control measures such as good handwashing and proper cough and sneeze etiquette are effective and important for prevention.
Hand hygiene is paramount, so wash your hands often with soap and water. Use enough soap, and make sure all parts of both your hands are washed. Spend at least 20 seconds washing your hands. If there is no visible dirt on your hands, an alcohol-based gel is also a good option. Stay home when you are sick, and avoid contact with other people. If you cough or sneeze, cover your mouth and nose with a tissue or with the inside of your elbow. Throw used tissues into a wastebasket immediately and wash your hands.
Physical distancing is advised in places with community transmission of the virus. Avoid crowded places and large gatherings, and generally keep some physical distance between you and other people.
For comprehensive information, including how to protect yourself against the disease, please visit the World Health Organization's (WHO) COVID-19 webpage. For updated technical information and details on the evolution of the pandemic please see WHO's COVID-19 situational report page.